Newborn screening for heart defects becomes mandatory
About nine of every 1,000 babies born each year have a congenital heart defect. Of those, about 25 percent have a critical congenital heart defect, which is the leading cause of infant deaths in the United States. To avoid severe symptoms, disability, or even death, these babies need the expertise of a health-care specialist within a few days after birth.
Because of this urgency, the Mississippi State Department of Health recently added pulse oximetry testing for critical congenital heart defects (CCHD) to the state's mandatory newborn screening panel.
"Of all the things we screen for, it makes sense to screen for heart disease because it's the most common congenital problem that you can be born with," said Dr. Mary Taylor, professor of pediatrics and chief of the Divisions of Pediatric Critical Care and Pediatric Cardiology.
The University of Mississippi Medical Center has been running the pulse oximetry, or pulse ox, screen on newborns since 2012.
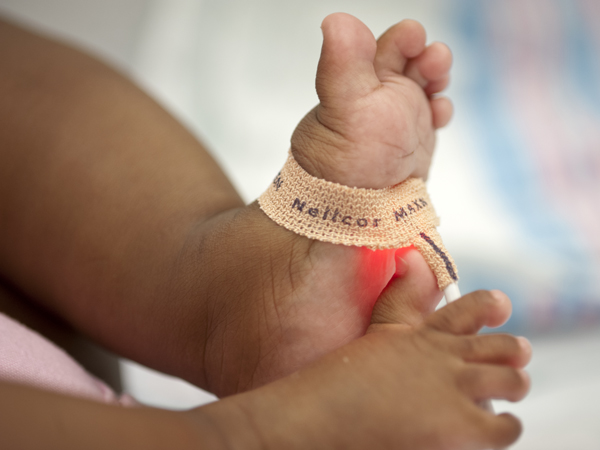
The inexpensive, non-invasive test uses sensors placed on a newborn's hand and foot to measure the percentage of hemoglobin in blood saturated with oxygen. Low levels indicate the baby may have a CCHD and alert the health-care team to run additional tests, conclusively identifying or ruling out a defect.

Savich
Dr. Renate Savich, professor of pediatrics and chief of the Division of Newborn Medicine, said many babies with heart problems look fine in the nursery because the ductus arteriosis - a blood vessel in the fetus that lets blood bypass the lungs and get oxygen directly through the placenta - is still open. That vessel closes during the first few days of life.
"With heart defects, as that vessel closes, there might not be enough blood going to the body or the lungs," Savich said. "Most of those kids, in the first or second day, will start showing some mild symptoms of not enough blood going to their body. It's hard to tell by looking at the baby. The babies normally would go home. They would get very, very sick and show up in the ER."

Taylor
A newborn ending up in the ER is exactly what Taylor and Savich hope to avoid with the new mandate. Requiring the test statewide will identify more babies with life-threatening defects, but more importantly, it will positively impact the health outcomes for these babies.
"The main thing is that they'll get to us in much better condition," said Taylor. "It's much better to know about it and to take care of it in advance."
That is exactly what newborn screenings are meant to do according to Savich.
"It's been going on for a few years and it has picked up some babies and again, it is a screen that's appropriate because you can find a baby with a heart problem, it's proving to be cost-effective and we can operate on these kids and fix them before they get really sick," she said.
Prior to the mandate to screen for CCHD, newborn screenings used a blood test to identify the most common genetic disorders. Like the pulse-ox screen, babies are tested shortly after birth so problems can be addressed quickly and hopefully lead a normal life with treatment.
Savich and Taylor both caution that some heart defects won't be revealed by a pulse-ox screening.
"It's a good test that will pick up most of them, but it doesn't pick up all heart defects and that's what people need to understand," Savich said. "Some things will still get missed."
They also agree the most important point is that the test will save lives.


