Gift of life: Transplants in 2016 at record high
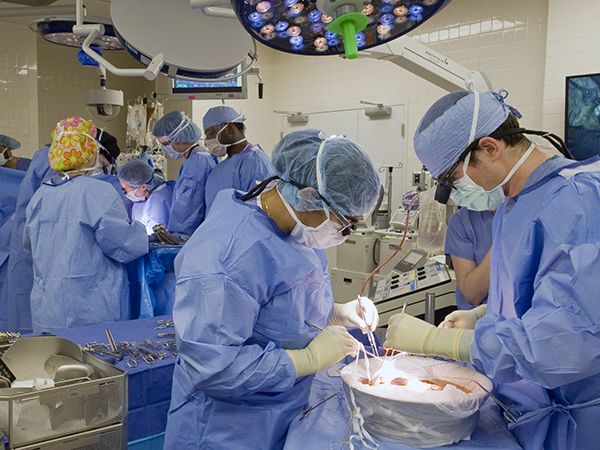
It's not unusual for the University of Mississippi Medical Center's abdominal transplant team to do a couple of surgeries in a 24-hour period.
But 11 over a long weekend, on top of trauma cases from the ED and other emergency surgeries vying for the Medical Center's 15 operating rooms?
Since the abdominal transplant program for liver and pancreas was rejuvenated in 2013, “hands down, that's the busiest run we have had,” said Dr. Mark Earl, associate professor of transplant surgery, who was on call the weekend of Oct. 27-30. The kidney transplant program was ramped up in 2011.
Earl and Dr. James Wynn, professor of transplant surgery, together handled the transplanting of 10 kidneys and one liver. All told, the transplant team performed 16 transplants over a seven-day period ending Oct. 30, Earl said.
“It's not uncommon to have days where we are very busy, but a seven-day period where we're doing multiple organs a day is very unusual,” he said. “This would be unusual for the biggest programs in the country.”
With several weeks to go, 2016 already is a record year in each of kidney, liver and heart transplant. “Our team at University Transplant has risen to that challenge many times, and this particular four-day stretch is a prime example,” Dr. Christopher Anderson, professor and chair of the Department of Surgery, said of the Oct. 27-30 run.

“There was no panic or stress — just the team doing its job,” said Anderson, an abdominal transplant surgeon.
Of particular note is the rise in heart transplants through the Division of Cardiothoracic Surgery. As of Dec. 1, 16 patients had received a new heart during 2016. That compares to just four hearts in 2013, increasing to nine in 2014 and 13 in 2015.
Three factors came into play, said Dr. Charles Moore, professor of cardiology. “We have a new head of cardiothoracic surgery, Dr. Anthony Panos. He's brought new enthusiasm for transplants and given us an additional transplant surgeon,” Moore said.
Also, he said, organ recovery in the state has increased. Thirdly, referrals of patients in need of a transplant are on the rise. “This allows us to increase our waiting list, and our transplants,” Moore said.
The 16 include Vicksburg resident Karen Gordon, 62, who got her long-awaited organ on Jan. 22, 2016. Her heart, weakened by a massive “widow maker” attack in 2010, was functioning at only 10 percent when a donor was found in Georgia and the UMMC team was able to maneuver around a snowstorm to go get the organ.
“They got me all prepared, and there's a whole lot to getting you prepared for surgery,” Gordon, a Vicksburg Realtor, said of the many people involved in making the transplant a go. “I can't say enough about my team. I had the best care.”
As of Dec. 1, the record number of transplants through the Division of Transplant and Hepatobiliary Surgery for 2016 included liver, 36; kidney, 136; and pancreas, six.
“It seems like every year, we're challenged with one or two periods like this, but I can't remember ever taking on 11 like we did,” said Bill Brister, nurse manager on 2 South, which has 10 beds dedicated to post-transplant care. The breakdown: four kidneys on Oct. 27, two kidneys on Oct. 28, four kidneys on Oct. 29 and one liver on Oct. 30.
“When I think about the whole weekend, it's why I love working here,” Brister said. “It's a group effort. You're only as good as your team.”
There wouldn't be any transplants if not for the many teams that come together to set them in motion, Earl said. “There's so much that goes on behind the scenes to pull off even one transplant,” he said. “There are a very large number of people involved. Any break in that chain can ultimately lead to the transplant not happening.”
The process begins when UMMC physicians get notification of an available organ from the United Network for Organ Sharing. The physician or surgeon determines whether a patient is suitable for the organ offered, and if so, will call one of the registered nurse transplant coordinators. That person calls the patient with the organ offer. If the patient says yes, events unfold very quickly.
A UMMC transplant surgeon travels to the donor and removes the organ or organs — or if the organ donor is at UMMC, removes them on site. The OR team is assembled and the surgery scheduled.
A vacant OR definitely is not a given, although room is always made. It's not unusual for all ORs to be booked between 7 a.m.-5 p.m., said Charles Wesley, assistant director of adult perioperative services.

The patient comes to the hospital, and caregivers do health checks and testing to make sure they're ready for a transplant. Hospital admissions and patient placement, in coordination with nursing staff, assign a bed to the patient. “We have great folks there. They know what we need, and they get it done to facilitate the process,” Earl said. “Sometimes they are up all night.”
“I have very seasoned charge nurses who know what beds are available and who can be moved,” Brister said.
When iced-down transplant organs are waiting, Earl said, OR availability is critical. “We want to minimize the organ cold time,” he said. “We did four of the kidney transplants Oct. 29. We never had to wait one minute. The team has to be committed to working hard to get the OR rooms turned over.”
Add to the OR mix Emergency Department trauma cases that could require surgery. “On that Friday night (Oct. 28) we had multiple gunshot wound victims, and we had another traumatic gunshot wound,” said Jason Zimmerman, director of nursing adult services.
When transplants are concluded, liver patients first go to the surgical ICU for several days, and kidney patients are placed in one of the 10 monitored beds on 2 South reserved for abdominal transplants, Brister said. Heart patients spend about a week in the cardiac ICU before going to 3 South, Moore said.
That October weekend, Brister said, he had to call in extra staff for 32-bed 2 South — and no one said no. “At one point, I had too many people willing to come in,” he said. “On a regular weekend, we generally have a staff of seven, but that weekend there were as many as 10 on a shift.”

Before they go home, patients get information on their medication regimen and how to care for their new organ. “My educator worked three of the four shifts that weekend,” Brister said. “It's a well-oiled machine. The front-line staff do an unbelievable job.”
“We are proud of the transplant system we have built here at UMMC,” Anderson said. “It can flex up and down to meet the needs of our patients. When times are busy and donors are available, our teams have risen to the occasion to ensure that we can always get our patients transplanted timely and safely.”
Gordon said she's doing well as she approaches the one-year anniversary of her new heart. “The biggest problems I've had are not from the surgery, but from just getting adjusted to my medications,” she said. “I'm blessed to have survived this. It's the most amazing gift.”
Especially in times of stress, Earl said, the Medical Center's transplant teams show their real colors.
“The surgeon gets all the hype, but that's just one piece of the puzzle,” Earl said. “It doesn't matter how well I cut and sew if everyone else isn't doing their job, and doing it well. This is completely a team sport.”


