Meet two new (robot) staffers in UMMC's COVID-19 testing lab

When you perform more than 1,300 repetitive moments with your wrists, fingers and hands during a regular work shift, it’s easy to suffer painful injuries that impact day-to-day existence.
But that’s what happened to some of the nine Molecular Pathology Laboratory team members who until recently hand-processed upward of 1,200 COVID-19 test specimens daily at the University of Mississippi Medical Center. UMMC processes virus samples collected at dozens of Mississippi State Department of Health testing sites, including the West Street Farmers Market off downtown Jackson. That’s in addition to samples from UMMC patients, its employees and students.
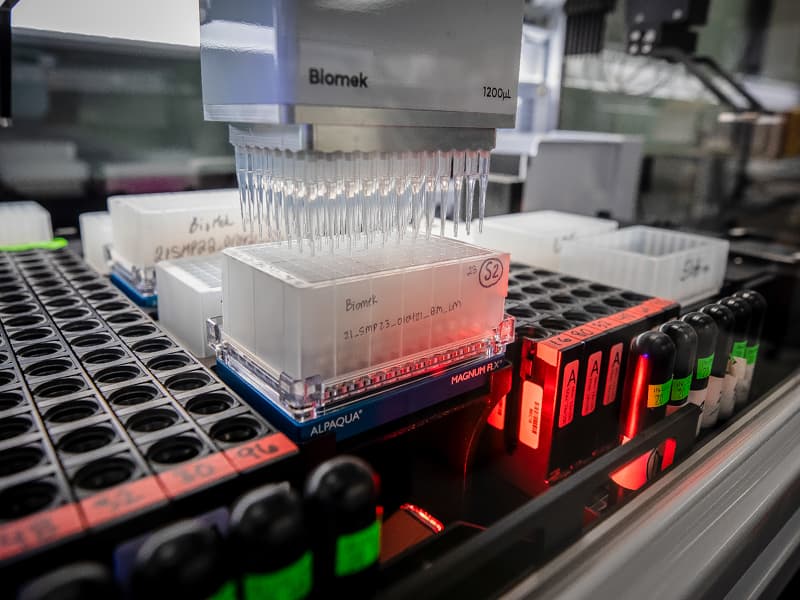

The installation of two new robotic computers, however, is transforming the step-by-step process of testing samples collected on nasal swabs. While humans must drive the testing to its conclusion, much of the manual work has been automated, said Dr. Sarika Jain, the lab’s director and an assistant professor in the Department of Pathology.
And although the equipment that went online Jan. 4 coupled with increased staffing will soon allow the Medical Center to double tests processed over a 24-hour period, it’s not just about the numbers, Jain said. “The biggest need for this instrument was to just continue doing what we are doing,” she said.
“The worry is that if the techs fall sick and are unable to work, we might not be able to do the testing that we’d been doing before we installed the new equipment.”
The two automated liquid handling robots work with the specimens and the reagents added to them to detect the COVID-19 virus. But when human hands do most of the work, there are more steps in the process, and it takes a lot longer to complete batches of tests.
Since April 14, lab team members have each performed, over and over again, a specific task required in the testing that detects genetic material in COVID-19 using a lab technique called real-time reverse transcriptase polymerase chain reaction – thus the test being dubbed RT-PCR.
“To make the process more efficient, it’s broken down into components,” said molecular pathology specialist Jake Johnston. “At the end of the day, you’re talking about a lot of stress on the hands.”

Specimens arrive in baggies, each containing a capped test tube that holds the nasal swab that was inserted into the patient’s nose to collect a mucus specimen. The tube also contains liquids – saline, or some other transport medium, Jain said.
“There’s a wrist movement for opening each tube, and most of the time, you have to twist it to remove it,” Jain said.
A technologist uses a pipette to suction liquid from each tube and place it on a large deep well plate, with each of its 93 wells serving as home to an individual liquid sample. Another technologist uses more pipettes to add reagents to each of the wells to extract RNA from the liquid and to cause the polymerase chain reaction needed for detection of COVID-19 genetic material.
Four extraction plates, holding a total 372 samples plus controls, were processed at a time, with 12 extraction plates typically completed daily, Johnston said.
“The wells are tiny,” said molecular pathology specialist Daniel Waltman. “It’s pretty strenuous on the hand and eye to add the reagents and then the samples to each of the wells.”
The testing robots arrived in early December, and Jain and her team spent several weeks validating that the machines would function accurately. That included testing how sensitive the machines are, checking for false positives and false negatives, and determining if the machines’ results correlate with results from the manual plating process.

“Some instruments are like an iPhone. You can pull it out of the box and it’s ready to go,” Waltman said. “With a precision machine, we had to do multiple calibrations and make sure the coding is specific to what we want to do.”
The robots make it possible to decrease use of plunger pipettes, Johnston said. “The techs still remove the swabs from each tube with a pair of disposable tweezers, but that’s their heavy lifting. The samples go directly onto the machine. The machine will put the samples into the wells on the plates.
“This doesn’t eliminate the human, but it changes what they have to do. The movements are more standard and what you would expect day to day.”
In addition to specialists Johnston and Waltman and lab manager Jennifer Phillips, the core testing team includes technologists Sara Kemp, Kinyetta Windom, Jackie Starrett, Luressie Jones, Reanna Perry, Eric Earnest and Jamie Jones. The laboratory is part of the Department of Pathology led by professor and chair Dr. Timothy Allen.
The immediate goal is to increase the number of samples run during a shift from 1,200 to 1,600 – and with the addition of a second employee shift, to double those numbers. That should significantly ease the current testing backlog, Jain said.
The second wave of technologists includes Jaquesha Harris, Amber Thomas, Amaani Belton, John Hankins, Kayla Reed, Lori Mosley and Tonia Taylor. “Hopefully, we can run the machines steadily and be in front of the game,” Johnston said. “Next-day turnaround is our goal. We want that so that people can make decisions about their health.”
There’s a lot of people chemistry in the lab, Waltman said. “This is a very dedicated, hard-working team that sacrificed Christmas to do their job. This doesn’t work as well as it does without a team that is willing to sacrifice and that is all about doing a good job.”

The laboratory is “the war room of the institution,” Allen said. “These people are extraordinary.”
Allen and his wife, Fran, have delivered home-baked goodies to the lab to show their appreciation. Allen on Jan. 4 received a thank-you note signed by the entire “war room” team. “It certainly rings true to the name,” the note read. “During World War II, battles would pause so that English troops could have a cup of tea. The same could be said for us. We pause for fresh air and fellowship over lovely treats!”
UMMC almost didn’t snag the robots, Jain said.
“We put the order in two months before we got it,” she said. “The day after we placed the order, the company told us if we hadn’t ordered it then, we would have had another several months of wait time. The whole country is looking for automation, and the whole country is looking at technician burnout and injuries.”
Today, her team sees “light at the end of the tunnel,” Jain said. “It’s amazing to see, even under these stressful conditions, that they are always smiling and talking to each other, and none of them have been diagnosed with COVID.”

