UMMC growing its robotic surgery program and necessary expertise
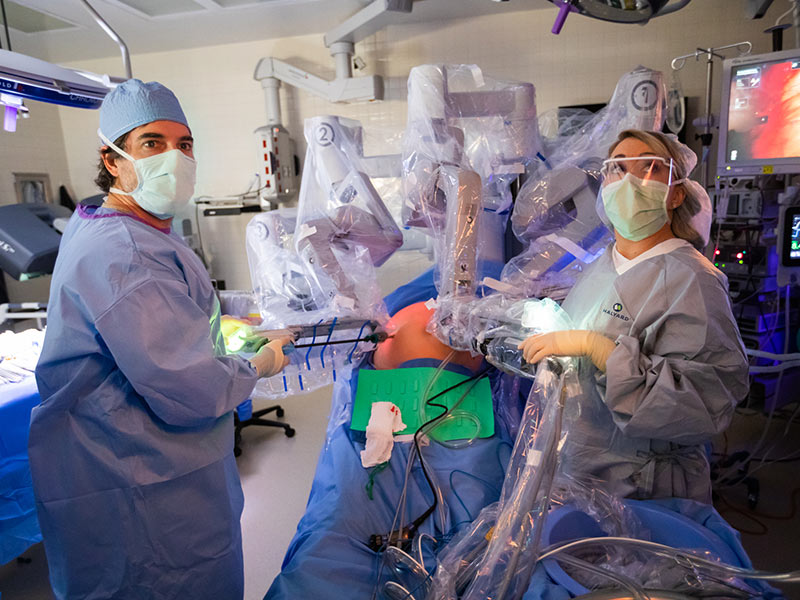
When Dr. Mark Earl performs a complex surgery to treat pancreatic cancer, his goal is to leave his patient not just cancer-free, but free from post-surgery complications and a lengthy recovery period.
So instead of making one large abdominal incision to remove the head of the pancreas, the first part of the small intestine, the gallbladder and the bile duct, Earl performs a more minimally invasive robotic procedure that calls for a number of much smaller incisions. “There are a couple of places around the country that have surgeons who do this laparoscopically, but it’s very rare and very hard,” he said.
“These are far and away done most commonly through a big incision,” Earl said of pancreaticoduodenectomy, a surgery more commonly known as a whipple procedure.
Earl is among a growing group of surgeons at the University of Mississippi Medical Center who perform complex operations via the use of a “robot” machine that allows more precision, flexibility and control than conventional techniques do. Robotic surgery has been performed for almost two decades, but its increasing sophistication has allowed expansion of its use in urologic, gynecologic and abdominal procedures.
Patients who are candidates for the robotic whipple generally go home a day earlier than those undergoing the more traditional surgery. “For an operation for gall bladder cancer, patients typically stay with us three to four days,” Earl said. “With robotic surgery, I’m sending them home typically the next day.”
Other advantages of robotic surgery include reduced pain and discomfort, faster return to normal activities, smaller incisions and reduced risk of infection, reduced blood loss, and minimal scarring.
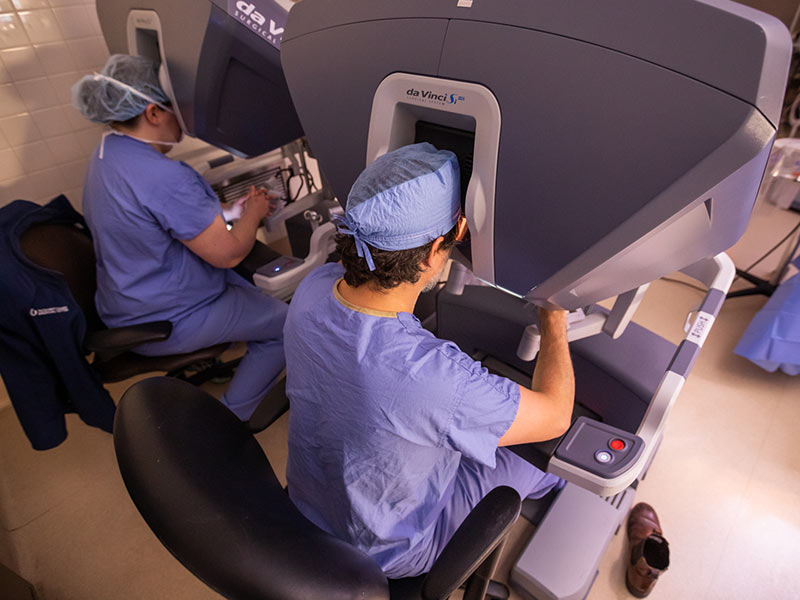
The most widely used robotic surgical system has mechanical arms with tiny instruments and cameras attached to them. The surgeon controls the arms while seated at a computer console table near the operating room table.
What the surgeon sees through magnifying glasses is a high-definition and enlarged 3-D view of the surgical site. The surgeon directs the robot’s arms in placing tiny metal tubes, or trocars, through small incisions at the surgical site. The trocars act as portals for passing miniature cameras and surgical instruments to the surgical site. To help position the trocars and perform the surgery, “we inflate the abdomen with carbon dioxide,” Earl said.
“I’m sitting beside the patient and control all the instruments being used on the patient,” Earl said. “There are two consoles so that we can have trainees who can learn and work. I sit at one, but have the ability to immediately take over.”
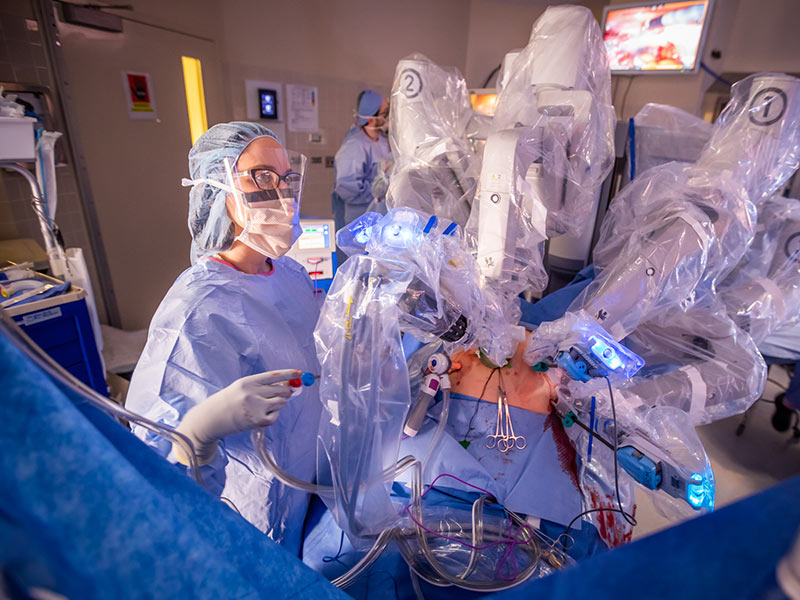
Not every patient is a candidate for robotic surgery over traditional approaches. And, surgeons have no business doing robotic surgery unless they are specifically trained. Earl, for example, trained at Carolinas Medical Center in Charlotte, N.C., “a very robust program. I watched a few cases and took a robotics course, and I also did online training,” he said.
“We have a robotic simulator in surgery and we practiced a lot on that, and a proctor from Baton Rouge came here and watched me as I did my first robotic surgery,” said Earl, who joined the UMMC faculty in 2012 as part of a transplant team recruited by Dr. Christopher Anderson, professor and James D. Hardy Chair of the Department of Surgery.
Since 2005, Dr. Mildred Ridgway has been performing robotic surgery for uterine and cervical cancer in addition to robotic radical and simple hysterectomies. Thirteen years later, “patient outcomes are still phenomenal,” Ridgway said.
“Gynecology and urology are the two specialties that pioneered the use of robotic surgery at UMMC,” said Ridgway, assistant professor of obstetrics and gynecology.
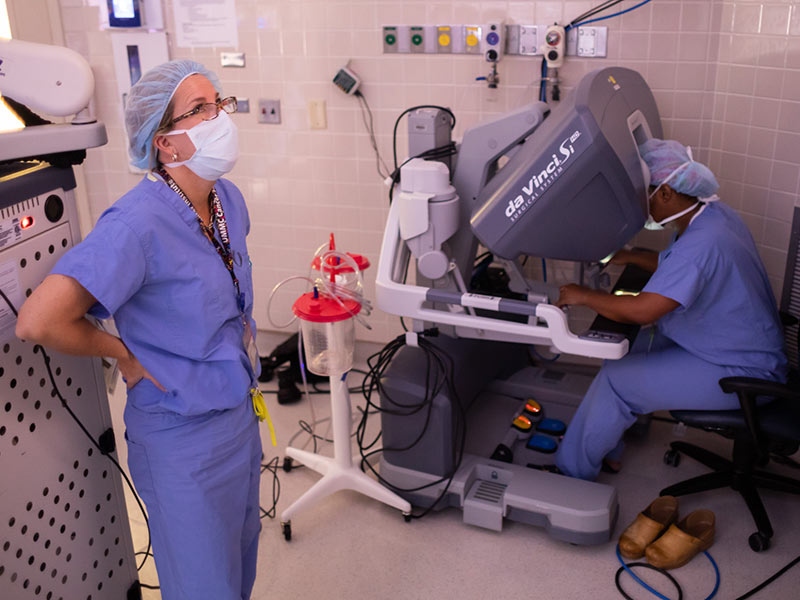
After making a number of tiny incisions at the surgical site, Ridgway said, she uses hand and foot controls to move the robotic arms that place the 3-D camera and dime-sized surgical instruments into tubes that travel through the incisions. Using the instruments, Ridgway excises the uterus, cervix and ovary. She also removes other tissue necessary in order to treat the cancer.
The Medical Center remains on the leading edge of robotic-assisted surgery for gynecologic cancers, she said. “I was one of the first people in Mississippi to do robotic surgery for GYN cancer, and we were pioneers nationally from the beginning. The volume of patients whose surgeries are done robotically is significant,” Ridgway said.
Today, she performs about 10 robotic surgeries a month, about as many as her busy schedule allows. All told, she’s completed upward of 1,500, which also includes procedures for advanced endometriosis.
Having a robust surgery program that includes the robot is critical to an academic medical center, Ridgway said. “If you don’t have robotic surgeries, you won’t be able to fill your residency programs,” she said. “It’s important to have it as part of your repertoire.”
Earl said one of the reasons he decided to train in robotic surgery was “to facilitate the training of our residents in doing complex surgery with a robotic approach.
“It’s taking hold more and more in colorectal surgery, but predominantly in hernia and anti-reflux operations,” he said. “Robotic hepatobiliary surgery is something that’s fairly new.”
General Surgery performs four to five very complex robotic surgery procedures a month, Earl said. Dr. Chad Huckabay, associate professor of urology surgery, performs two to three robotic procedures a week. Fifty to 60 percent are for prostate cancer, about 20 percent for kidney tumors and cancer, and the rest for benign kidney conditions including blockages of the ureter, Huckabay said.
The benefits to patients are great, he said.
“Kidney surgery typically requires a pretty large and painful incision,” said Huckabay, who came to the Medical Center in 2010 and trained in robotic surgery during his fellowship. “There’s a big advantage to robotic surgery because the incisions are very small. It’s also nice because you can see blood vessels a lot better with magnification. Typically, you have far less bleeding risk because of the magnification, and because you use very tiny instruments that do tedious work.”
Huckabay and other surgeons often explain to patients the differences between robotic surgery and other popular minimally invasive surgeries, such as laparoscopic or laser procedures. “Some patients ask if a robot is going to do their surgery,” Huckabay said. “I tell them that it’s a surgical instrument, and the surgeon is in control. And, you have more than that surgeon. Typically at this university, there’s a surgeon at the patient’s bedside, likely a resident, helping to operate the robotic arms and laparoscopic instruments that are used as well.”
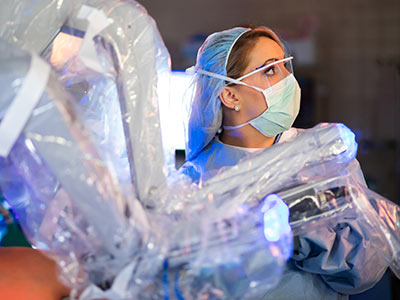
Robotic surgery does come with potential risks, including hemorrhaging caused by lacerations, unintended retained foreign objects, and damage to surrounding tissue.
“Patient safety is always key,” Earl said. “Patients with a number of prior abdominal operations aren’t good candidates for the robot, and patients that I know will be extraordinarily complex, such as those needing the rebuilding of major blood vessels, are done with open surgery because the risk of bleeding is high.
“I won’t compromise the safety of patients, or the quality of operations,” he said. “I want patients to be comfortable and to have the quickest recovery that they can.”
The future of robotic surgery at the Medical Center is ever-changing. “With time and advances in the robot, what you will start seeing is instead of surgeries being done with four or five tiny incisions, it could be done with two, and in some cases, maybe one,” Huckabay said.
“I’m learning new things all the time,” Earl said. “The next phase for me is major liver resections. It’s just finding the right patients.”

