Forging students into physicians: The residency reality

Completing a medical residency is like running a marathon or flying a plane.
“You don’t know what it’s like until you’ve done it,” said Dr. Meagan Mahoney, who graduated last month from the surgery residency program at the University of Mississippi Medical Center.
After four years of medical school, graduates must undertake another three or more years of rigorous specialty training involving long and late hours, high-stakes decision-making and stress. They are called residents because, at one time, their teaching hospitals were also their homes.
“A residency is an apprenticeship,” said Dr. Mark Earl, associate professor of surgery, transplant surgeon and program director for the general surgery residency at UMMC.
As with many professions and trades, a physician’s “apprentice” often arrives with enthusiasm and excitement, along with some expectations that are affirmed or abandoned over the course of time.
To illustrate how these notions stack up against reality, six people agreed to give their takes: two residency directors – of general surgery and obstetrics and gynecology; two recent residency graduates; and two incoming residents, or interns, all at UMMC.
FIRST, AND SECOND, THOUGHTS
OB-GYN
Dr. Ashley Surles of Madison; intern, OB-GYN; [her husband Dr. Bret Surles is a first-year pediatrics resident at UMMC]:
“I know about the long hours. It’s just as hard as getting through medical school, but as a resident you’re doing what you love. Our families have been through medical school with us. They know what to expect.
“We’ll just put our heads down, work hard and come up for air when we can.”

Dr. Rachel Riley of Clinton; June 2018 residency graduate, OB-GYN:
“The hours were longer than I expected. It’s not only being physically tired, but you’re emotionally tired as well. You deal with fetal deaths and talking to patients about it. It’s having to make on-the-fly decisions. These are things I didn’t know would be so hard.
“The intern year was probably the hardest. Really early hours, a steep learning curve. It was a big adjustment, from being a fourth-year medical student to becoming a doctor.”
Dr. Elizabeth Lutz, assistant professor of OB-GYN, OB-GYN residency program director:
“As a medical student, I thought it was all pap smears and delivering babies. In medical school, you go through specialty rotations, but it’s hard to get a feel for what it’s like day-in and day-out for any field.
“If I could pick one quality for a successful resident in any field it would be grit. Are you going to have a bad day and come back the next ready to work?
“What makes OB-GYN different from many other specialties is that it’s both medical and surgical. I tell residents, ‘I really have to trust you to give you a knife and let you cut open a patient I’m in charge of.’”
SURGERY
Dr. Colton Lee of Poplarville; intern, surgery-preliminary:
“I’m nervous about the amount of responsibility; I can’t say I’m just a medical student anymore. It’s on me when it comes to patients. But I’m excited about that, too, and about being around like-minded people. Doing what I came to medical school to do.
“My goal is to be comfortable and competent in operating, and realize my limitations. The personality of a surgeon is thinking you can fix almost anything. I want to be able to know when to ask for help.
“I’m grateful that I had rotations in other specialties as a medical student, but I’m glad that now I get to take care of surgical patients. I get to hang out with surgeons, pediatric surgeons. I consider them superheroes.”

Dr. Meagan Mahoney of Columbus; June 2018 residency graduate in general surgery:
“If you’re a medical student thinking you want to do surgery, you don’t have to be 100 percent sure, but you should be at least 99 percent sure.
“The struggles we go through can get you down. The trauma cases stick out. Car wrecks. Something unforeseen by the patients. The specific cases I remember are the ones that went bad. The ones we couldn’t help.
“Several times I thought, ‘Why did I go into this?’ The thing that always brought me back was seeing the patients, especially their families.
“You see the fear in their eyes; they don’t really understand surgery. It’s being able to tell them, ‘It’s going to be alright.’”
Dr. Mark Earl, associate professor of surgery and general surgery residency program director:
“Most medical students probably have a good idea of what they are getting into. The part that probably surprises them the most is the intensity of the work, and how sick the patients really are.
“I believe a lot are surprised at the difficulty in making decisions – when oftentimes they have to do it. Many decisions may seem easy or obvious to someone who doesn’t have to make them.”
FIRST LOSSES
SURGERY
Dr. Meagan Mahoney, general surgery residency graduate:
“The intern year was really hard. Dr. Kenneth Vick [professor of surgery] called me after a patient died – the first death during my residency.
“He told me how he lost his first patient. He said, ‘You never get used to it; you just get better at dealing with it.’”

Dr. Mark Earl, general surgery program director:
“During the five years of general surgery residency, a large part is learning to operate. That is probably the easiest thing we teach. The art of surgery is developing good judgment – which operation is appropriate for a patient.
“Probably more important is realizing which patients you cannot help. Surgery may not help some patients, and that’s a skill that takes years and years to learn.”
Dr. Colton Lee, surgery intern:
“I don’t know how to prepare for it yet. I haven’t processed that. I need to start thinking about it.
“But it’s probably going to be a pretty tough day.”
OB-GYN
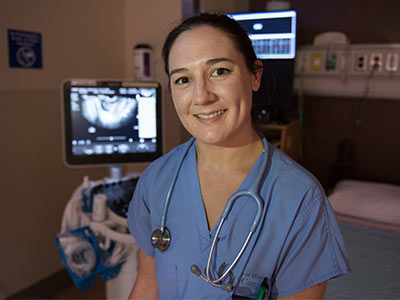
Dr. Ashley Surles, OB-GYN intern:
“One thing that I have been nervous about was how to tell a patient that she’s lost a child. I’ve asked everyone how they deal with that.
“It’s sitting down with them and telling them in plain language what has happened. It’s letting them grieve and go through the process. It’s telling her, ‘It’s not something you did, and we’ll do everything we can to take care of you.’
“The focus of a residency is to learn, but it’s also to treat patients as something more than instruments to learn on. It’s a tough balance to think about losing someone you care for. I can look to those above me to see how they deal with it.
“And we will do all in our power not to lose anyone.”
Dr. Rachel Riley, OB-GYN residency graduate:
“We had a patient who needed an emergency hysterectomy at 4:30 in the morning; she had two liters of blood in her belly due to a uterine rupture. She had been seen in clinic where it was noted the baby had died in the uterus, requiring admission for induction and delivery.
“But there are also what seems to be hopeless cases that we are able to fix. There was a diabetic patient with a difficult and late delivery who had to be induced. Her baby weighed 10 pounds, 15 ounces and had a shoulder dystocia [abnormal position or size].
“It was one of the scariest moments I had in residency. The delivery caused an injury to the baby’s arm, but otherwise the baby was OK, and the mom did well.
“Afterward, though, I was shaking. The nurses hugged me. They thought the baby was going to die.
“You become so attached to the patients, especially the oncology patients. You see them go through so much, and it’s so rewarding when you see them go into remission. But there are those whose cancer keeps progressing and you feel like there’s nothing you can do.
“It’s nothing you do wrong. But these are the only times, maybe, when I feel defeated.”

Dr. Elizabeth Lutz, OB-GYN residency program director:
“People think, ‘I’m going to deliver a baby; I’m going to be happy every day.’ My own mother believes we have a job where we are happy every day.
“There is so much joy in what we do. But there are moments of sadness, too. I tell residents, ‘Those are the moments when you, as a doctor, are making the most difference.’
“Before residents ever deal with a death for the first time, they should ask themselves what they would do if this happened.
“When a patient gets bad news, a resident or medical student should observe the way the attending physician handles it: What do you say to the patient? What’s the appropriate body language?
“Doctors tend to believe they can fix almost anything. Sometimes you can’t fix it; you just have to take care of your patient.”
LAST WORDS
SURGERY
Dr. Mark Earl, general surgery residency program director:
“Ask for advice; two heads are better than one. Never be in a challenging situation alone. Be it in the ICU, the OR, the emergency room, anywhere. Rarely are things certain.
“If you ever find yourself certain about a decision, be very careful.”
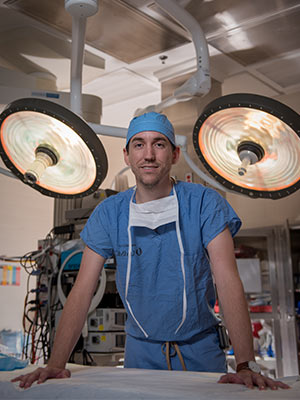
Dr. Colton Lee, surgery intern:
“I expect to be a different person in five years; just like I was after four years in medical school.
“One of my coping mechanisms is my dog Remington [a 3-year-old Dalmatian]. He keeps me grounded and mentally sane.
“Also, I already know some of the other interns. We’re going to be in this together. On my bad days, I can reach out to one of them. And I hope that on their bad days they can lean on me.”
Dr. Meagan Mahoney, general surgery residency graduate:
“As a resident, I probably grew up. I’m less naïve about the world.
“As a medical student I wanted to save the world. You’re not going to save the world. But you can make changes; you can help people, which is a good enough reason to keep at it.”
OB-GYN
Dr. Ashley Surles, OB-GYN intern:
“I believe the only time residency should be competitive among those inside the program is if you’re competing for a fellowship spot. Otherwise, you need to work as a team day-to-day.
“When I was a medical student, the residents here were helpful because of the interest I showed. They let me be involved.
“We’ll be stronger as physicians if we lift each other up.”
Dr. Elizabeth Lutz, OB-GYN residency program director:
“Interns should learn to rely on each other. It gives them that that strong sense of not being alone. It’s a good feeling knowing that others are going through this, too.”
Dr. Rachel Riley, OB-GYN residency graduate:
“One patient owned a cake shop with her mother; she made me a bunch of sweets and brought them to clinic one day.
“During her second pregnancy, another mom asked me to be her child’s godmother. When a patient shows appreciation, it makes it all worthwhile. You feel like you made a difference.
“I tell people I may be emotionally tired, but I can’t imagine doing anything else with my life.”

