Little hearts, many experts: Children’s Heart Center grows to meet needs

Kingston, who has had four open-heart surgeries to correct a congenital heart defect, and Gabbi and Jharad, who as infants had heart transplants, are among the many patients of Children’s of Mississippi’s Children’s Heart Center.
“We are growing, because the need is growing,” said Dr. William Moskowitz, chief of UMMC’s Division of Pediatric Cardiology and co-director of the Children’s Heart Center.
The number of Children’s of Mississippi pediatric cardiologists caring for the little hearts in the state has never been larger.
The Children’s Heart Center, which will have a new home in the University of Mississippi Medical Center’s $180 million pediatric expansion, now has a record 15 pediatric cardiologists. The latest additions include Dr. David Weiland, who specializes in electrophysiology; Dr. Stephanie Ghaleb, whose expertise is in cardiopulmonary stress testing, and Dr. Himanshu Adlakha, who will join Dr. Brad Troutman at Children’s of Mississippi’s specialty clinic in Biloxi.
Moskowitz is excited about the changes now and in fall 2020, when the children’s hospital addition opens.
“Having a comprehensive program, which is what we have, with a dynamic team, and now to have a new state-of-the-art facility coming – this is what we cardiologists pray for,” Moskowitz said.

About one baby in every 100 is born with a heart defect, and these can range from mild to critical.
The progress that has been made in pediatric cardiology and cardiothoracic surgery, though, is nothing short of phenomenal, Moskowitz said.
About 50 years ago, most children born with serious congenital heart defects, or CHD, died in early childhood.
“Years ago, about 95 percent of these kids were not going to reach adulthood,” he said. “Now, more than 90 percent survive into adulthood.”
Reflecting those advances, the Adult CHD program at the University of Mississippi Medical Center has seen an increase in patients of more than 700 percent since its opening in 2014.
“It’s incredible,” said Dr. Mike McMullan, chief of cardiology and leader of the program. “The technology and surgical techniques have improved so much that now there are more adults with congenital heart disease than children.”
Kingston, 7, of Brandon, was born with hypoplastic left heart syndrome, a condition in which the left side of the heart does not fully develop in utero. Kingston started first grade this fall, about three years after his last surgery.
“He’s doing great,” said his mom, Liz Foster, project manager of Children’s of Mississippi’s Safety and Community Outreach program. “He’s spent the summer at trampoline parks and swimming pools. This past year, he played baseball and is turning out to be a pretty good player!”
TRANSPLANTING HOPE

The Medical Center’s pediatric heart transplant program, started in 2011, has had “a tremendous success rate,” said Dr. Avichal Aggarwal, medical director of the program. “In the past five years, we’ve had a 100 percent success rate.”
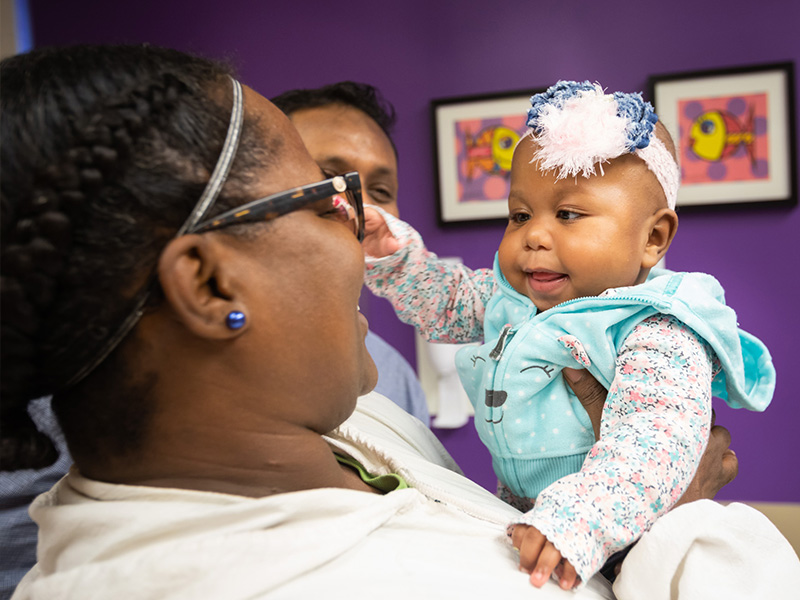
Among Aggarwal’s patients are two of the youngest children to ever have heart transplant surgery at UMMC, Jharad, now 2, of Meadville, and Gabbi of Bassfield, who’s nearing 2.
The children were each about 3 months old and in need of new hearts. Today, both are thriving toddlers.
“They’re both doing great,” Aggarwal said.
He’s made sure of it. Each of his heart transplant patients’ families are given his cell phone number with his request for a text each day. “I don’t care if there are no changes. For the first year, I want that text every day so we know how the patient is doing.”
REDUCING RISK
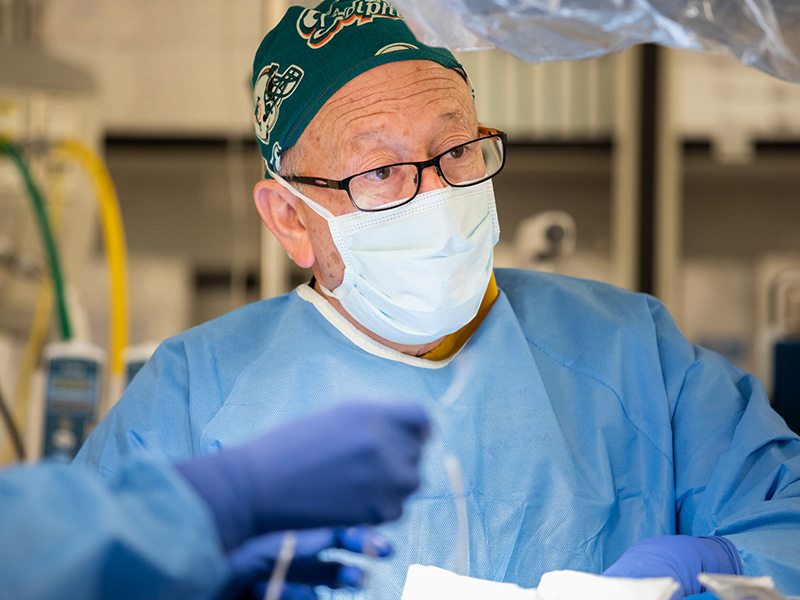
In the specialty clinic area of the new children’s hospital tower, treadmill and bicycle stress tests will be available, as will evaluation of heart and circulation function through exhaled gas analysis.
“Put together with a stress echocardiogram, we can better evaluate the heart’s function, not only at rest but during exercise,” Moskowitz said.
New portable blood pressure monitoring will allow for better evaluation of patients, Moskowitz said. “It allows us to really follow them outside the clinic, to see how their cardiovascular systems perform when they are at rest and also when exercising, to know when to intervene and how they respond to therapy.”
According to Mississippi Department of Health statistics, more than 40 percent of Mississippi children are either overweight or obese, which can create heart conditions such as hypertension. The American Academy of Pediatrics has reported that children with high blood pressure are more likely to continue to have hypertension as adults.
“We are seeing patients with early coronary artery disease risks at a very young age,” Moskowitz said. “We work to not only get their blood pressure down but also to reduce their risk profile with dietary and lifestyle modification.”
SURGICAL EXPERTISE
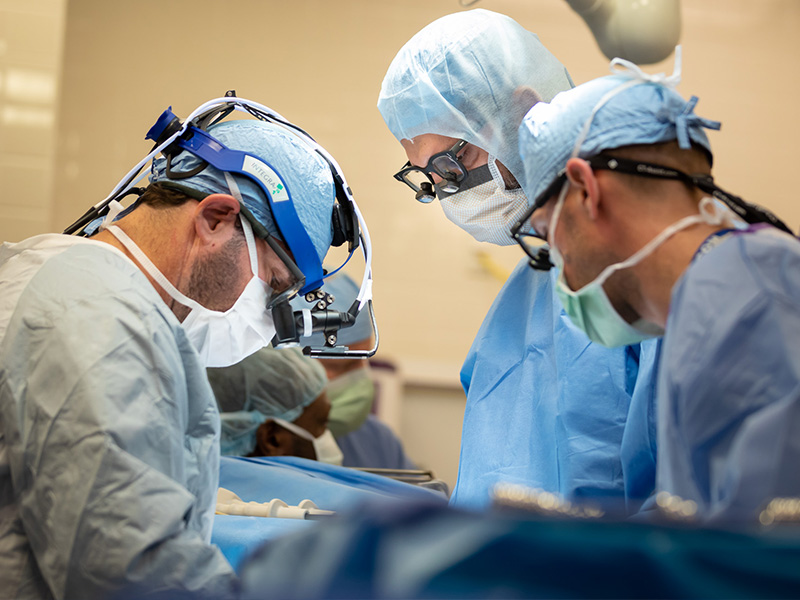
Batson is the only place in the state where pediatric heart surgery is performed, and Children’s of Mississippi physicians and surgeons have a record that rivals the nation’s leading children’s heart programs. “Dr. Ghanamah trained under me at Emory and Children’s Healthcare of Atlanta’s Congenital Heart Center of Georgia, one of the largest and most comprehensive congenital heart surgery programs in the country,” Kogon said. “He is an excellent surgeon and can perform the entire spectrum of congenital heart surgery.”
Prior to coming to UMMC in 2017, Kogon was chief of pediatric cardiothoracic surgery at Children's Healthcare and director of adult congenital cardiac surgery at Emory University.
Ghanamah was drawn to children’s heart surgery because of the difference it can make in a child’s life.
“These children, after surgery, are able to lead full, healthy lives,” Ghanamah said. “To be able to help children reach their full potential, sometimes through only one surgical procedure, is awesome.”
One of those children is Bailey Sanderford of Hattiesburg. A patient of Dr. Makram Ebeid since she was an infant, the 17-year-old has had about 15 catheterizations and five heart surgeries. Her latest, performed this summer, was an 11-hour procedure to replace two valves.
“When we first met Dr. Ebeid, it was at the entrance of Batson,” said her father, Lance Sanderford. “He was waiting at the door for us, and the Children’s Heart Center has been with us since.”
Bailey’s surgery, though lengthy, shows the level of care offered. The most complex surgery performed in congenital heart disease is the Norwood operation, which carries a survival rate of 85 percent. The division’s surgeons have performed eight Norwood heart operations in the past year, with a 100 percent survival rate.
In the Society of Thoracic Surgeons database, the program’s mortality rate is 1.7 percent, significantly below the national average of 3.2 percent.
“We have a phenomenal team of surgeons,” said Moskowitz, “and their outcomes are fantastic, with support of an outstanding team of nurses, critical care physicians, anesthesiologists and many others.”
NEW HOME
Once the seven-story children’s hospital expansion is open in fall 2020, the space where the intricacies of children’s hearts are seen through sonography will become office space for pediatric cardiologists and fellows in training.
Meanwhile, instead of having to travel deep into the Medical Center, patients and their families will be able to have their outpatient visits in the new multidisciplinary specialty clinic, part of the expansion.
“This will be easier and more convenient for patients and their families,” said Moskowitz. “It will be a state-of-the art facility, and it is being built with collaboration in mind, so that patients can see multiple specialists and have multiple tests if necessary during the visit without having to leave the building. And parking will be immediately adjacent to the building!”
The tower will also include 10 additional operating suites, 88 private neonatal intensive care rooms, and increases in number and size of pediatric cardiac intensive care spaces. The Children’s Heart Center performs more than 400 surgical procedures each year.
The need to transport medically fragile patients across long distances will be eliminated, and private waiting areas for families are a part of plans.
Inside the expansion’s outpatient pediatric specialty clinic, state-of-the-art equipment will be available for diagnosing, treating and monitoring patients. Collaboration will be enhanced in the new area, allowing cardiologists to work with experts in other disciplines as members of a medical team for complex patients.
“We have a great program now,” said Moskowitz, “but when this new expansion is open, we will have a program that will be among the best in the country.”


