Quality care, quality performance means better outcomes
Published in News Stories on October 22, 2015
Caregivers at the University of Mississippi Medical Center strive daily to reduce injuries to patients that are associated with their care, a number that nationwide is as high as 27 percent of Medicare patients annually.
Those adverse events - among them patient falls and safety or medical missteps that result in injury - can mean a prolonged hospital stay, permanent harm to the patient, a life-sustaining intervention, or even death.
Today's efforts aren't enough, however. Zero preventable harm and improved quality outcomes, such as better patient satisfaction and lower readmission rates, are tough goals that can be reached incrementally, said UMMC Chief Medical Officer Dr. Michael Henderson.
Breazeale
As the nation observes Health Care Quality Week, “it's time for UMMC to jump on the bandwagon and further improve the care we provide to patients,” said Amanda Breazeale, the Medical Center's manager of performance improvement.
“At UMMC, the quality focus is on setting targets for improvement over current baseline performance levels so that we take hard, but achievable, incremental steps towards zero preventable harm and high level performance on publicly reported outcomes,” Breazeale said.
Initiatives that are under way include:
- Error prevention training for all 10,000 employees.
- A revitalized hand hygiene campaign driven by front-line staff.
- Reducing patient falls by using the Hester Davis Falls Risk Assessment Scale to predict anticipated falls.
- Leadership rounds to hear what both patients and front-line caregivers have to say.
- Improved documentation of care given and the severity of the diseases treated.
- An added emphasis on ownership of the work, with shared accountability and responsibility.
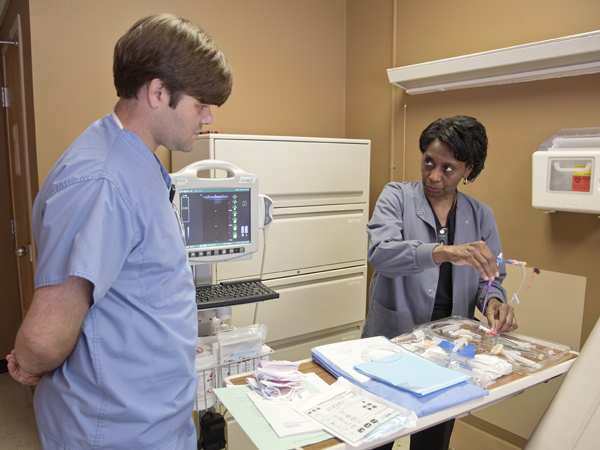
Among the patient harm events caregivers strive to prevent are hospital-acquired infections. Training is an important front-end deterrent to cleanliness issues that can result in an infection. That's one lesson driven home this week by Carolyn Thomas, a member of the Medical Center's PICC (Peripherally Inserted Central Catheter) Team.
Thomas is training registered nurse Brandon Rowell, who came to UMMC about two months ago to join the PICC Team. He hasn't yet placed in a patient a central catheter line, a small tube inserted into a vein to gain short-term or long-term IV access for both inpatients and outpatients.
“Everything must be sterile,” Thomas told Rowell as she talked him through the procedure, not with an actual patient, but instead with necessary equipment, including an ultrasound machine to locate a patient's veins. “We do not want them to get any kind of infection from us placing this line.”

Henderson
Quality Week, Henderson said, “brings into focus the work and the people who drive improvement in patient safety, outcomes and experience in health care. Here at UMMC, quality improvement is right at the top of our strategic agenda.
“First and foremost, it means that we want all caregivers to understand and participate on improving safety, outcomes and satisfaction for our patients,” he said. The Medical Center is giving them the tools through opportunities for improvement, set and focused goals, and the formation of teams for projects that will engage front-line caregivers, he said.
“Quality Week becomes a rallying point for all hospitals across the country to focus on these issues and set their agendas to do the right things for their patients,” Henderson said.
There have been significant improvements in U.S. health care over the past few years, driven in part by the nationwide Partnership for Patients Initiative, which aims to save lives by reducing hospital-acquired conditions by 40 percent and improving transition of care, thus reducing readmissions, by 20 percent.
Those goals were met nationally between December 2011 and December 2014. Broken down, that's an estimated 92,000 harms prevented, with an estimated cost savings of $988 million, the American Hospital Association says.
Decreasing patient harm also decreases costs, Henderson said. The national Centers for Medicare and Medicaid Services in 2014 penalized more than 700 hospitals with high harm rates by withholding 1 percent of all Medicare payments they take in during fiscal 2015. At UMMC, that meant the loss of about $900,000.
The specific focus areas for quality improvement for 2016 are spelled out in the new scorecard on the Clinical Intranet. “The baseline measurement and targets for improvement are currently being defined and locked down so that everyone can see how we perform and where we want to get to,” Henderson said. “All caregivers are stakeholders in achieving this goal for patient safety, outcomes and experience.”
“We can, and will drive change and all be proud of how this really helps our patients,” Breazeale said.



