Epic’s vital sign capture saves caregiver time

Published in News Stories on March 13, 2017
When Lesley Colwell provides care for children in Batson Children's Hospital's Pediatric Intensive Care Unit, she spends a little more time at their bedside than she could a week ago.
An Epic program that automatically gathers patients' vital signs from their monitors debuted in the PICU March 7. As a result, front-line caregivers no longer have to manually enter numbers on 10 vital sign variables - including heart rate, blood pressure, respiratory rate and oxygen saturation - into a computer.
Instead, Epic captures the information in a “vital signs complex flowsheet,” that is ready to be viewed within a minute after the information has been recorded.

Colwell
“This will decrease the amount of time nurses sit at a computer to input data,” said Colwell, a nurse manager. “All you have to do is look and click 'validate.'
"Talk about a time saver!”
The “go live” of the Epic integration program in the PICU follows its implementation about a year ago in the Neonatal Intensive Care Unit, the adult Intensive Care Units and cardiovascular holding, or CVH. Before the implementation, nurses in the NICU manually entered vital signs as often as every 30 minutes to an hour, according to nurse manager Carla Gill.
“We're getting ready to do the same thing with ventilators," she said. "That's a biggie.”
Heath Prejean, a senior interface analyst in the Division of Information Systems, said the Epic patient device integration is a team effort. The team is exploring more integrations, including bedside infusion pumps.
“We're adding a hook across the network," Prejean said. "It captures the information and reels it back into Epic.”
When nurses view the vital signs fed into Epic, they hit “validate” to officially enter the vital signs into the patient's chart, Gill said. If a baby is crying and his or her heart rate is elevated, “a nurse might not validate it because it's not truly accurate,” she said.
Physicians will be able to see both unvalidated and validated data on the flowsheet.

Gill
“If you're manually doing it, you might have a tendency to flip numbers and not realize it,” Gill said. “This was a little bit hard to get used to: Nurses are used to entering their own numbers. But it does streamline the process.
"If you've got a really sick baby or a lot going on, you don't have to manually enter anything. You're just clicking one button instead of filling out a lot of drop-down boxes.”
“We're definitely glad to have it,” said Dena Peoples, CVH nursing shift supervisor at University Heart. The CVH primarily cares for outpatients, but also inpatients who have just had particular heart procedures. “As many procedures as we monitor, this frees the nurses up to do patient care.
“It has saved a whole lot of manually entering vital signs - printing them off monitoring stations and entering them one at a time.”
It's especially useful for looking at trends and baselines, Peoples said.
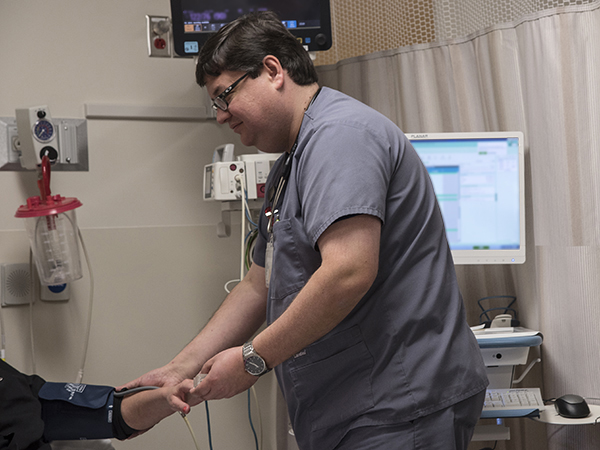
Nurse John Lentz visits with a patient while her vital signs are being fed into the new medical records system.
Don Horn, nurse manager in the cardiac ICU, said the program is a boon to the care of critically ill adults.
“You will have a few glitches here and there, but it's a time saver,” said Horn, who noted readings from ventilators and bedside dialysis machines also are recorded.
Device integration “improves the work flow to make sure we are not only accurately recording vitals, but doing it in a timely fashion,” Prejean said. “Doing as much device integration as we can around the hospital is one of our missions.”
The ability to automatically collect data in Epic, “is a dream we heard about when we first got Epic," Colwell said. "It finally has come into fruition.”


