Diabetic no more: Patient gets state's first isolated pancreas transplant

Ask brittle diabetic Nancy Smith why she opted for a pancreas transplant, a rare procedure not without risk or potentially devastating complications, and she’ll tell you about her heart.
There’s her son Carruth, an 18-year-old high school senior. There’s daughter Braeden, 23, a college graduate and preschool teacher.
“They’re amazing,” the Jackson resident says of her children. Carruth copes with the challenges of Asperger’s Syndrome, a form of autism, and a rare neuropsychiatric disorder associated with strep infections.
“They made the decision easy. I want to watch them continue to grow, and to be around for all the major life events to come,” Smith said. “He needs me, and so does she. Nobody is like a mama.”
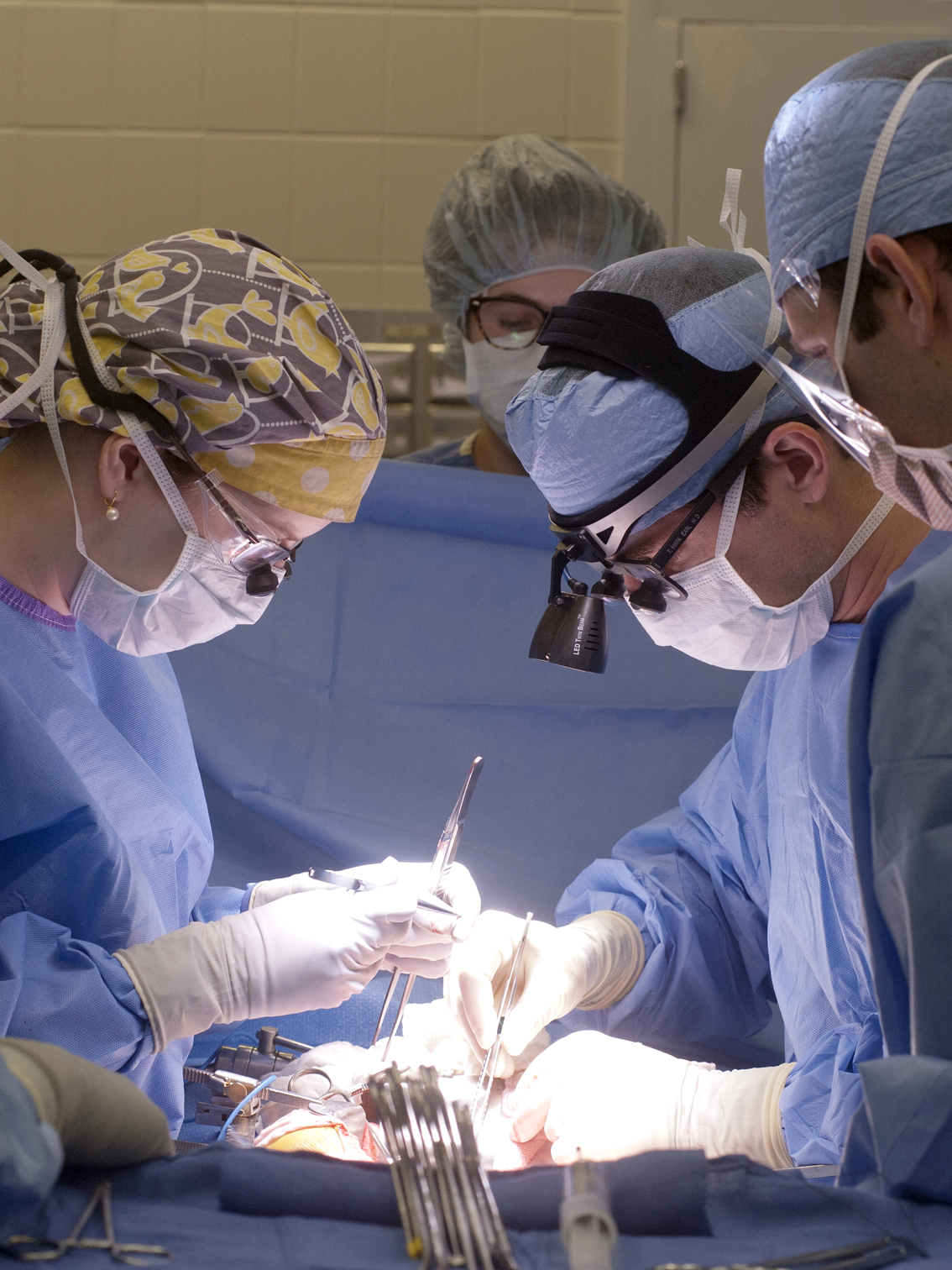
On Sept. 30, Smith became the first person in the state to receive an isolated pancreas transplant at the University of Mississippi Medical Center – not the more medically common combination of a pancreas and kidney, but a pancreas alone. “It’s an incredibly rare procedure,” said Dr. Mark Earl, an assistant professor of surgery at UMMC, who performed the transplant and whose expertise includes all aspects of liver and pancreas surgery and transplant.
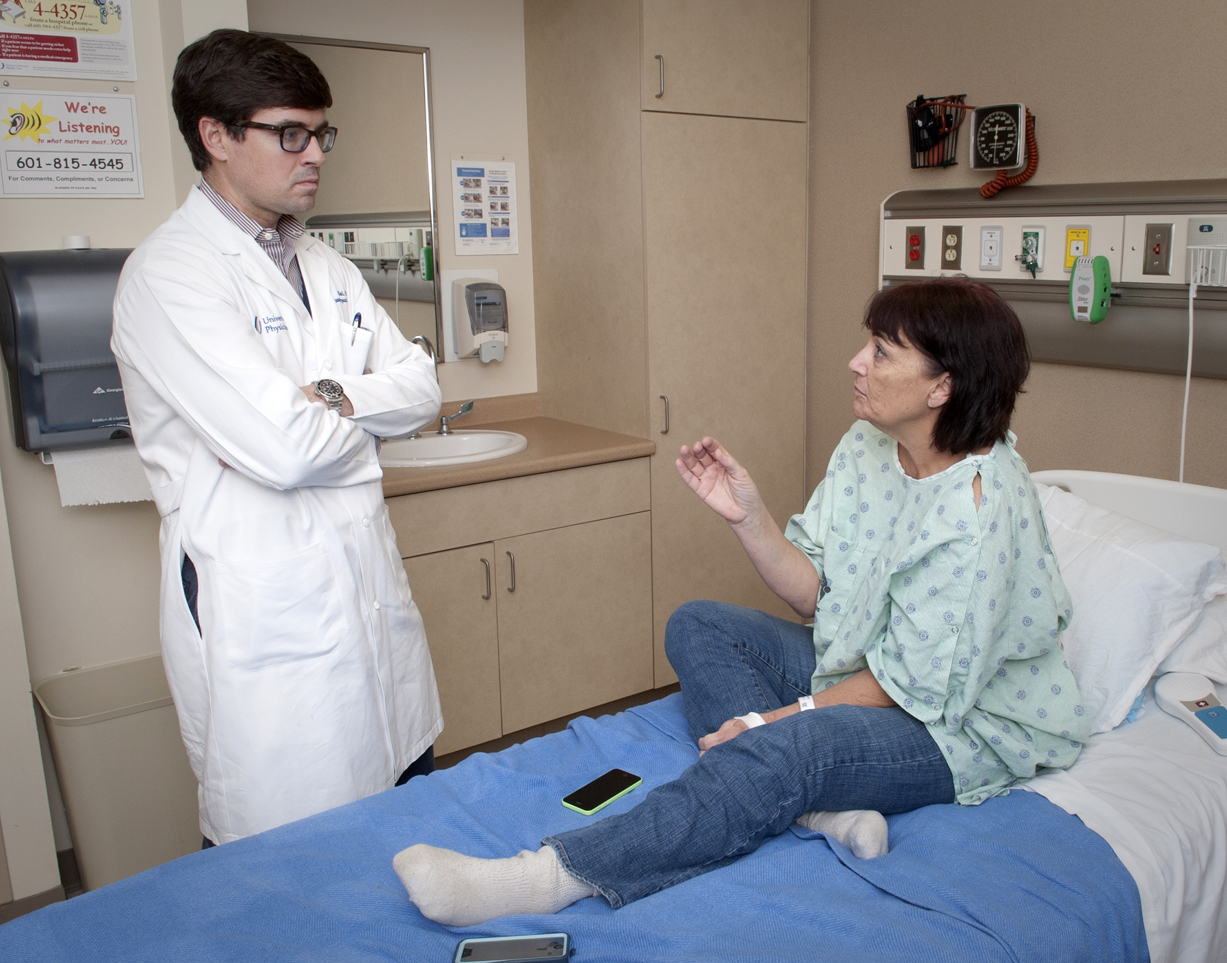
“It’s especially rare for someone who has no kidney failure, but has other life-threatening complications from type 1 diabetes,” Earl said. And, he said, the surgery marks the 10th transplant of a pancreas at UMMC this year, putting its transplant program on par with other acclaimed programs in the Southeast.
Diagnosed with juvenile diabetes, 52-year-old Smith said she and her doctors knew it would be a matter of time before she’d need a transplant. She lost sight in one eye. Her neuropathy was worsening. Quality of life was waning.
Because Smith’s pancreas wasn’t producing the hormone insulin and couldn’t regulate her blood sugar levels, her blood sugar was unpredictable and would drop without warning, causing her to pass out. “Low blood sugar can be immediately life threatening. You pass out, and if it doesn’t come back up, you can die,” Earl said.
“Because Nancy is a Type 1 diabetic, the insulin-producing cells in her pancreas had been killed by her own immune system,” Earl said.
During a three-hour operation, Earl left her native pancreas alone; it worked well except for that one potentially fatal flaw. The donated pancreas he positioned into her abdomen produces crucial insulin, which stimulates cells to absorb sugar from the blood.
Before the surgery, Smith had tried to do all the right things: Frequently exercise. Watch her diet and weight. Pray. Try not to fret about the future.
“If I could stay calm and not worry about things as much, that would help,” Smith said. “I wouldn’t be here today if I didn’t exercise like I do.”
But as her health continued to deteriorate, Smith in July 2013 secured a place on the transplant waiting list at Ochsner Medical Center in New Orleans. It was right before UMMC’s transplant program began performing pancreas-kidney procedures.
“They had to take me off the waiting list at Ochsner because I couldn’t find anyone who could go to New Orleans and stay there three months with me,” Smith said.
The timing could not have been better.
“It was ironic,” said Smith’s sister-in-law, Terri Gillespie of Jackson, who happens to be UMMC’s chief nursing executive officer. “She came over to the house and said she wished UMMC would get approval for a pancreas transplant. I said, ‘Oh, my gosh. That happened yesterday! ‘ ”
In January, Smith met with Dr. Kenneth Kokko, an associate professor of nephrology and member of UMMC’s transplant team. “Dr. Earl came in, and he said, ‘You’re going to be the first person to receive a pancreas transplant, and if there was any person who needed a pancreas transplant, you’re it,’ ” Smith remembered.
On Sept. 24, Earl called her: A donor pancreas had been located. She grabbed the bag that had been packed for months and headed to UMMC, only to find out that the pancreas wasn’t viable for transplant. “We got back into the car, and Nancy said, ‘I feel like I had Braxton-Hicks contractions and I went to the hospital to have a baby, and I got sent back home,’ ” said her sister, Janie Robbins of Ridgeland.
“Carruth was so sad when I came back home,” Smith said. “He didn’t say a word. He just put his head on my shoulder. Braeden was bummed, but positive that all things happen for a reason.”
Just days later, Earl summoned Smith again with news of a potential pancreas. She hurried back to UMMC, donned a hospital gown, and counted down the hours before surgery in a patient room, Gillespie and Robbins at her side.
Earl stood at her bedside and detailed the risks: There would be a 30 percent chance she’d have to go back into surgery the first week. There was a 10 percent chance the blood supply to the new pancreas could become blocked during the first six weeks.
“There’s about a 20 percent chance of rejection, but in the overwhelming majority of folks, the transplanted pancreas lasts a long time and they are done taking insulin injections,” Earl told her.
“I’m the overwhelming majority!” Smith told him.
As Smith, Gillespie and Robbins waited for word from Earl on the pancreas’s viability, they shared a laugh over memories of Smith owning a cupcake store in the face of diabetes. And, they somberly contemplated the fact that because someone died, Smith could have a better and longer life.
“I’m overwhelmed,” Robbins said. “You know someone’s going to be giving us the greatest gift.”
“If I can just have five more years ….” Smith said, willing back her tears. “I just need a little more time.”
When they thought a transplant was imminent a week earlier, Gillespie said, “I felt elation, and then did a lot of praying.
“Often times with a transplant, if it’s an unexpected death, it gives a donor family a feeling of closure – that it wasn’t all for nothing,” said Gillespie, who spent many years as an emergency room and recovery nurse.
Earl sent Smith home just five days after she got her new pancreas.
“Everything’s a miracle,” said Smith, who wants to help people understand the importance of organ donation. “When I woke up from surgery, I didn’t have diabetes. Now I can see shapes and some other things out of my right eye. I’ve never had this many normal blood sugars this many days in a row.
“I cannot imagine having anyone else in charge,” she said of Earl. “He has given me quality of life back.”
Said Earl: “She’s not just recovering from surgery. She’s recovering from years of diabetes. But with her energy level and the rate she is recovering, we’re going to have to slow her down, rather than tell her she needs to get moving and start living life.”
He and his staff are watching Smith carefully, taking frequent bloodwork and making sure she regularly checks her blood sugar. “That is one of our best markers for pancreatic function,” he said.
As Smith’s recovery continues, Earl said, so does her prospect of a long and healthy life.
“I want her to get 20 more years completely free of diabetes. That’s the whole point. If this wasn’t the point, it wouldn’t be worth the risk,” he said.
“My hope is that she goes on to die of something else as a very old lady.”


