New guidelines: lower blood pressure for better health
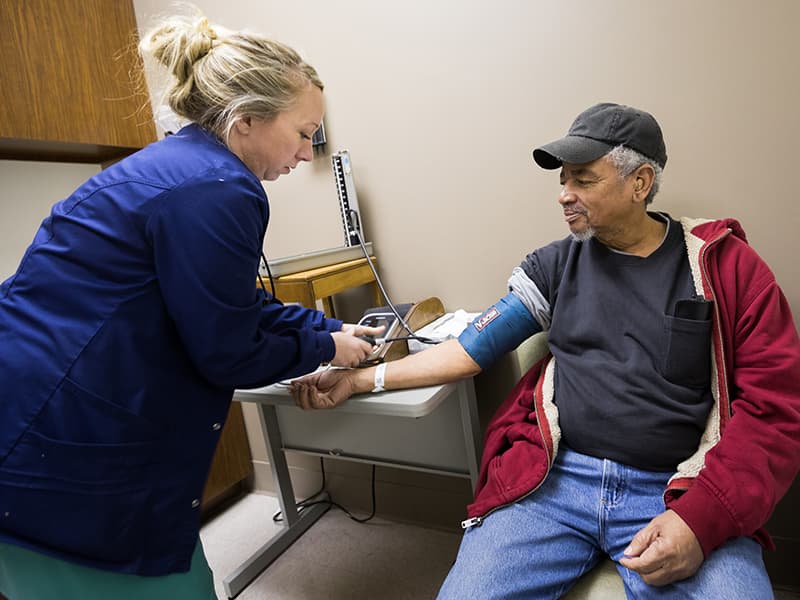
On November 13, more than 30 million Americans developed high blood pressure.
Two of them are relatives of Dr. Dan Jones, which he discovered while measuring blood pressures at his family’s Thanksgiving celebration.
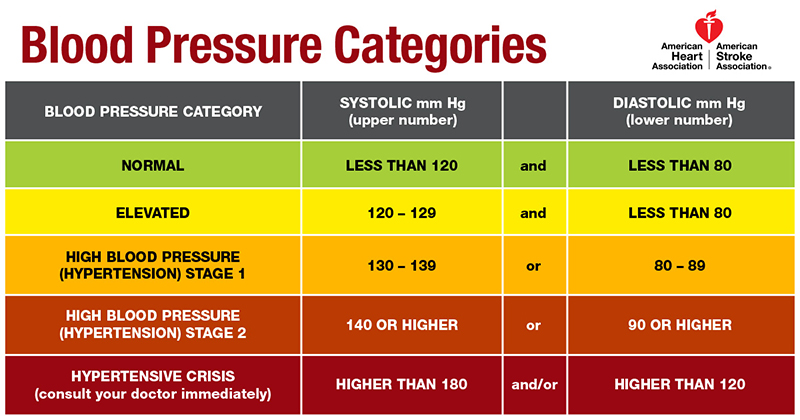
That’s because the American Heart Association and the American College of Cardiology recommended to change the threshold for diagnosing and treating hypertension to 130 over 80 mmHg, lowering the previous standard of 140 over 90.
The change didn’t happen overnight. Jones, professor and interim chair of medicine and co-author of the new guidelines, said the panel of 21 experts reviewed more than 900 studies conducted worldwide to inform their decision.
“What we have known for some time is that elevated blood pressure increases a person’s risk for cardiovascular disease,” said Jones, former president of the AHA. “What we didn’t know is where this risk begins.”

“There is enough evidence to say with certainty that lowering blood pressure to this level has substantial benefits,” Jones said.
Known as a “silent killer,” hypertension is a chronic medical condition and risk factor for not only cardiovascular but also renal disease. The AHA and Centers for Disease Control and Prevention estimate that hypertension caused or contributed to more than 360,000 deaths nationwide in 2013 and costs Americans more than $46 billion each year.
Announced at the AHA’s Scientific Sessions 2017 meeting in Anaheim, California, the new 130 over 80 guideline raises the proportion of Americans with high blood pressure from 32 percent to 46 percent.
Prior to the new guidelines, Mississippi had the nation’s second highest rate of adult hypertension at 42.2 percent, according to the CDC. By lowering the threshold, Jones said more Mississippians are at risk. An exact prevalence under the new numbers is not yet available.
Jones said one important effect of redefining hypertension as 130 over 80 is that people will receive treatment earlier. It could also prevent people from developing dangerously high blood pressures in the first place.
Hypertension has multiple causes, including diet, exercise, obesity, genetics, smoking and stress. Most of these factors can be modified to help lower blood pressure.
“We are blessed with a wide variety of effective anti-hypertension medications and the knowledge that lifestyle changes can improve our health,” Jones said. However, “controlling blood pressure isn’t easy for some people.”
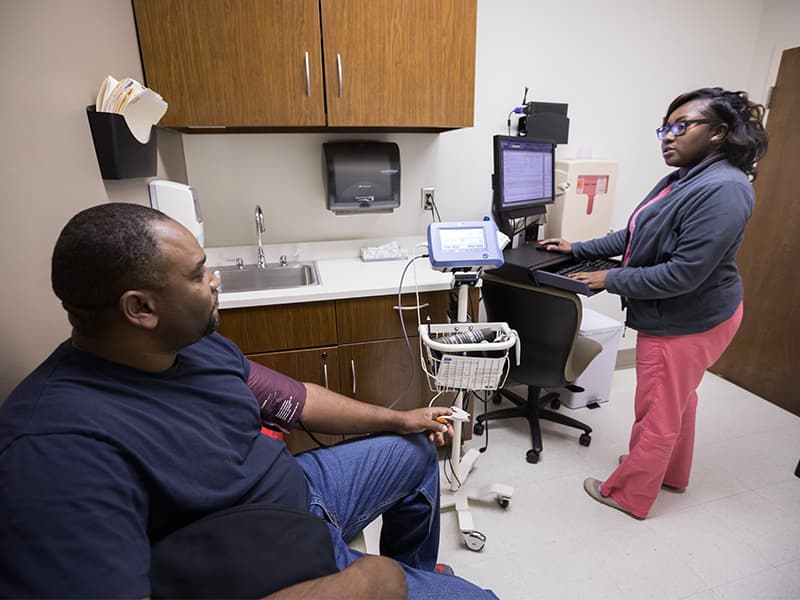
About 70 percent of people treated for hypertension achieve their goal. The new guidelines will drastically increase the number of people requiring an intervention.
“Based on these recommendations, the prevalence of hypertension has increased from 70 million individuals to 103 million,” said Dr. Joey Granger, professor of physiology and biophysics and a hypertension researcher.

“More aggressive lowering of blood pressure requires more drugs,” said Granger, who serves as dean of the School of Graduate Studies in the Health Sciences. “Severe hypertension patients may take multiple medications simultaneously to meet their goal. Since we have this new target, we need more research into treatment options.”
UMMC faculty conduct extensive basic research into the origins and treatment of hypertension, Granger said. Several labs study potential targets for new kinds of anti-hypertensive medications. Others have extensive focus on hypertension in pregnancy and end-organ damage associated with high blood pressure.
Jones said those most affected by the change will be adults older than 65 and younger than 45. Among younger men and women, hypertension prevalence is expected to triple and double respectively, according to the guidelines.
The good news is that most of the people with newly-diagnosed hypertension can be treated with lifestyle changes. In their guidelines, the AHA said diet, exercise, weight loss and limiting alcohol intake can lower blood pressure by 4 to 11 mmHg, enough to bring many of the new stage 1 hypertension patients back into a healthier range.
Jones said that some clinicians and patients may be frustrated by the new guidelines. This could be particularly true when it comes to treating patients who experience adverse reactions to anti-hypertensive medications or older people who may not tolerate lower blood pressure well.
“Guidelines are guidelines,” Jones said. “A clinician needs to use their knowledge and experience to decide how low of a blood pressure their patient can tolerate.”
However, Jones said, the extensive review suggests that nearly “anyone can have their blood pressure lowered using standard treatments without undue harm.”
For 2018, Granger is planning meetings to help educate local clinicians on the new guidelines.
“These are very important changes,” said Granger, chair of the AHA Council on Hypertension. “It’s been 13 years since these guidelines have been updated.”
Jones said he is “pleased with new programs” UMMC has developed to help its employees and patients achieve healthy blood pressures. These include the Department of Preventive Medicine’s Everyday Wellness program and clinical studies on primary prevention.
“We want people to live long, healthy lives,” Jones said.
---
Learn more about hypertension here.

