Laser therapy restores hope to patients with persistent brain tumors
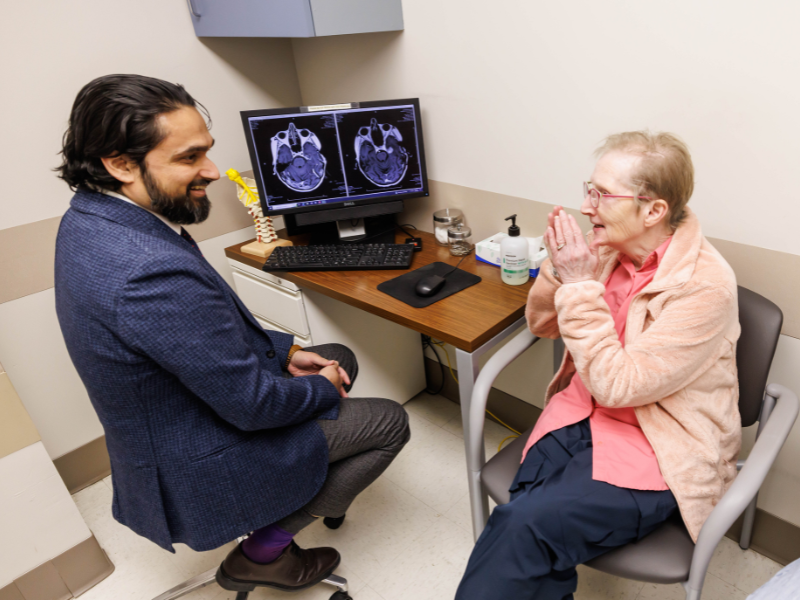
A decade ago, Georgia Pritchard of Sturgis was diagnosed with stage four breast cancer. But by the time she found out, the cancer had already spread from her breast to her spine and hip. Soon, the cancer spread to her brain, causing a tumor to grow.
“I had stage four cancer for years,” Pritchard said. “They treated it and treated it. Eventually, some of the places in my body began to heal. But a lot of the time, it would come back. It was very discouraging for a long time, but then the results started getting better. Slowly, but surely, all the cancer in my body healed— except in my brain.”
Over the past decade, Pritchard has undergone various treatments to eliminate the brain tumor, including whole brain radiation, four Gamma Knife radiosurgeries, an open craniotomy and several rounds of chemotherapy. But, through it all, the cancer persisted.
For patients with recurring tumors like Pritchard, UMMC now offers a new neurosurgical procedure that comes as a welcome alternative.
The procedure, called laser interstitial thermal therapy, is a minimally invasive surgical technique that uses a small laser to destroy, or ablate, unhealthy brain tissue. It can be an effective treatment option for recurrent brain tumors like Pritchard’s, tumors formed deep within the brain and radiation necrosis (a rare complication of cranial radiation therapy).
“This technology is the most advanced anywhere in the state,” said Dr. Omar Chohan, associate professor of neurosurgery and director of surgical neuro-oncology. “It’s going to be very good for our patients.”
Not only does laser ablation therapy open a new avenue for cancer treatment in the state, it is also a new option for some patients with epilepsy caused in areas of the brain too risky or inaccessible for open surgery, Chohan said.
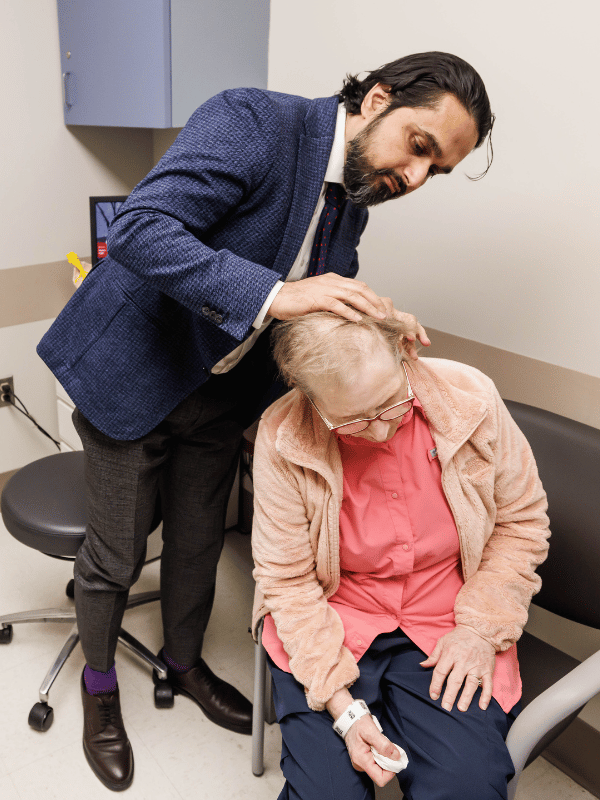
He reported that Pritchard’s tumor is already shrinking. “It’s hollowed out and I think it looks great,” he said. “We have cautious optimism. This one tumor has been a challenging problem for many years now and we have thrown everything at it.”
Pritchard said she almost lost hope after her years-long cancer battle. “I just can’t believe it,” Pritchard said. “I had about given up a couple years ago, but I decided I’m not going to quit. And now this has come along, and I feel hopeful that I may finally beat it,” she said.
LITT consists of two consecutive procedures totaling about an hour. In the first procedure, a laser fiber is placed into the affected area of the brain with the help of a high precision robot. Following a CT scan to ensure the proper placement of the probe, the tumor is removed using a technique called “MR thermography.” The laser is activated inside an MRI machine, where the magnetic field causes it to heat up and destroy the unhealthy tissue.
“This part only takes about 10 minutes,” said Chohan. “Thermal ablation kills cells by heating up the tissue beyond a certain temperature. So, anything less than 43 degrees is considered ‘the safe zone,’ meaning the tissue won’t die at that temperature.”
He said the ablation process is highly targeted and controlled. “You can put safety zones around the tumor, so the ablation doesn’t go beyond a certain area. You can contour—so in lesions that aren’t perfectly symmetric, you can use multiple probes to cover, or contour, that area. And you can stop the laser at any time.”
After the probe is taken out, the small 3.2-millimeter cut is closed with a single stitch. Then, another CT scan is done to make sure there's no bleeding. Chohan explained that the patient stays in the hospital overnight to be discharged the next day.
The procedure is intensely multidisciplinary, requiring synchronization of everyone involved, including radiation oncology, medical neuro oncology, neurosurgery, radiology and the technology specialists.
“It’s a very technologically intense process, but it’s very simple on the patient,” said Chohan.
Another benefit of laser ablation is that it aids in recovery by opening the barriers in the brain for medical therapy, such as chemotherapy and radiation therapy. And, as the tissue is ablated, proteins called antigens are released which help program the immune system to fight off the cancer.
“We are the only center that offers this technology in the entire state, and this opens the door for a lot of patients,” said Dr. Chohan. “If they are too sick to undergo a traditional craniotomy, the surgery is too risky, they’ve failed surgery, chemotherapy, radiation—previously patients who would have had no other choice—they have been given this option now.”
Pritchard said she is grateful to everyone who had faith in her healing. “It’s unbelievable,” she said “I want to honor the people who prayed for me and the doctors and everyone who pulled for me to get better. Something just told me to keep fighting. And that’s what I did.”


