Experts plan to call the shots this flu season
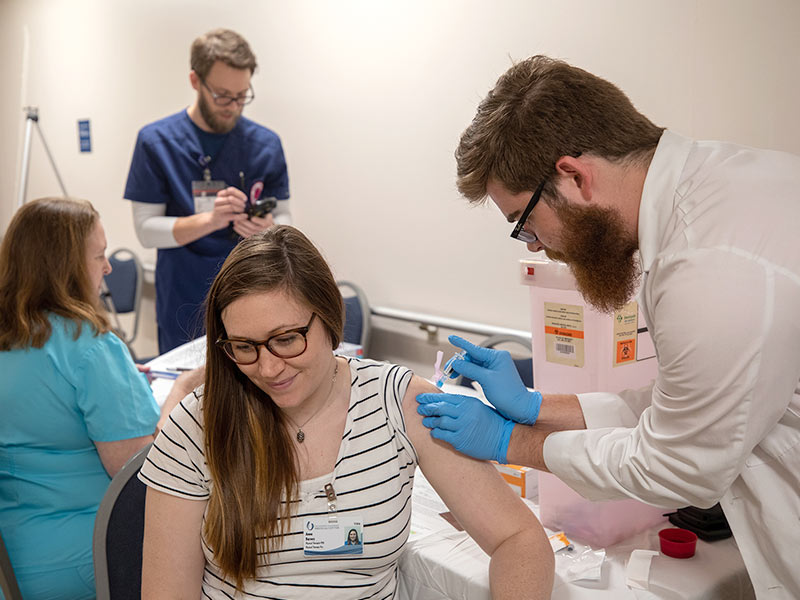
When Australia coughs, America listens.
“Australia’s flu season can be a precursor to ours in the United States,” said Jason Smith, manager of emergency services at the University of Mississippi Medical Center.
“We’re watching the trends and patterns to see how they may correlate here in the U.S. and how that may affect the Medical Center. In Mississippi, the flu season has already begun.”
At UMMC, the impact of a major flu epidemic on operations is comparable to that of a ruinous tornado’s aftermath, or a “security event involving a weapon,” Smith said.
No wonder, then, that UMMC coordinated not only a flu vaccination “blitz” on Tuesday, but is also staging an information offensive to allay the anticipated assault from the bug. Because the news from Australia is not good.
Already in the midst of spring, that upside down world endured a worrisome flu season during the virus’ peak, including the winter months of June to August.

“They’re ending their season now,” said Sheila Fletcher, director of infection prevention at UMMC. “They started seeing cases earlier this year than usual.”
Fletcher’s infection prevention team is helping spread the word about ways to prevent spreading the flu; the tips are for visitors, as well as employees: use hand sanitizers, wear face masks when appropriate, cover your coughs and sneezes.
This work involves, among other things, putting up educational posters and wall “clings” around the campus, not least of all in the areas of pediatric care. The number of influenza-associated deaths for the 2018-2019 flu season – 61,200 in the United States – included 138 children, as reported by the Centers for Disease Control and Prevention.
As the CDC also noted, the previous flu season may not have set a record for severity, but it was the longest in a decade. Officially, it started Oct. 1, 2018 and ended in May.
Influenza is no respecter of calendars; it does not care if it’s hot outside. But as colder weather sets in, people tend to huddle indoors, and are more likely to accidentally shake hands with the flu.
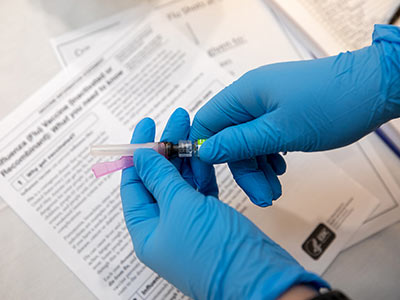
Right now, the Medical Center is focused on “prevention and surveillance,” said Smith, who has discussed with Fletcher ways to curtail the contagion across campus. “It’s not just the health care side that’s affected; it’s the entire institution.” A preparedness exercise being developed for November will bring that point home to the Medical Center’s leadership, not only to those in health care, but also to those in areas such as Human Resources, supply chain and more.
For physicians like Dr. John McCarter, preparations include trying to make sure vendors of ventilators and other breathing equipment will be able to cope with extra orders if needed. It means being able to set aside Day Surgery and certain post-surgery units for a surfeit of flu patients “if there is a shortage of beds,” said McCarter, associate professor of emergency medicine.
The risk of a shortage is most likely at season’s peak, which, in Mississippi, is usually late in the fall or early winter. But it could last into March or later, Smith said. “Last year we had a relatively mild flu season; but we expect it will be extensive this year.”
To sidestep surprises, Medical Center experts turn to the Mississippi State Department of Health and the CDC to help track the flu’s progress, not just in the Jackson area, but also across the state and even the southeast region.
“We accept patient transfers from hospitals throughout the state daily, which could increase our flu season load,” Smith said. “We do see an increase in transfers when the flu hits.”
To cope with that load, it’s vital that employees protect themselves. “If health care providers miss work because they’re sick with the flu, that puts a further strain on the health care system,” Smith said.
Coming to work while sick is no good either, McCarter said. “Medical professionals are focused on wanting to help, so they can lose awareness that they may be helping to transmit disease. But they should stay home.
“For those who must take up the slack, don’t look at it as having to do more work; look at it as, ‘Oh, boy, I’m avoiding getting sick because my friend stayed home today.’”

In addition to heeding the flu prevention tips, stopping, or at least mitigating, the spread of the flu depends largely, of course, on getting the vaccine. “Employees, staff and students are required to get the flu shot,” Smith said, “and we encourage them to have their family members vaccinated also; if they have to leave work to take care of sick loved one, that also strains the system.”
This season’s vaccine, as usual, is meant to protect against four strains, McCarter said. “We’re pretty confident that two of the parts of the vaccine are well-matched to the strains we’re expecting to face.
“But, even when there isn’t a perfect match, people who get the vaccine and then get the flu are less likely to get pneumonia, are less likely to be hospitalized and are less likely to die.”
For patients with other, existing diseases, getting a flu shot may be even more critical. “We have a very high disease burden in this state – asthma, diabetes, coronary artery diseases and more,” McCarter said “In all of those situations, having the flu worsens outcomes.
“With coronary artery disease, within a week of getting the flu, patients are six times more likely to have a heart attack than at any other time in their life.”
Such patients may have to resort to the emergency room – if they can’t get an appointment with a primary physician within 48 hours of the onset of symptoms: fever, chills, sore throat, dry cough, muscles aches, McCarter said.
“If you can’t get a timely appointment and have, say lung disease or diabetes, or if you’re pregnant, then we want to see you in the emergency room.”
Otherwise healthy people, however, should stay home and/or see a primary care doctor. Because unnecessary emergency room visits also burden the system.
“If you can go in for an office visit, that would increase the capacity of the ER and you might be seen in a more timely manner,” Smith said.
Telehealth is another option, he said. “You can virtually communicate with a provider, who could potentially send in a prescription to your pharmacy if needed.”
For his part, McCarter has one more word of advice; really, four: “Don’t smoke. Don’t vape. They increase complications and make you more likely to get the flu.
“Also, a vaping-associated lung injury on an X-ray looks much like influenza, so how would I know what I’m dealing with?”

