UMMC fills neurology gap with first-time inpatient telehealth evaluations
When Michael Bustin’s right side lips went numb and his speech became slurred March 25, his wife Ruth rushed him to the emergency room at South Central Regional Medical Center in Laurel.
“I wasn’t worried, but she was,” said Bustin, 76, who works 10 hours a day, five days a week at Masonite, a door manufacturer.

What followed was a battery of tests to determine if the temporary numbing was caused by a neurological problem. Bustin was admitted to the hospital, and on March 27, that Monday, he saw Dr. Juebin Huang, associate professor of neurology at the University of Mississippi Medical Center.
“Your MRI looks normal,” Huang told Bustin after greeting him and his wife and asking Bustin a series of questions. Bustin told Huang he was waiting to receive an ultrasound of his heart, and hoping to get clearance to go home later in the day.
“We checked the vessels in your neck, and they look quite clear,” Huang said. “This could have been a mini-stroke – a TIA (transient ischemic attack).”
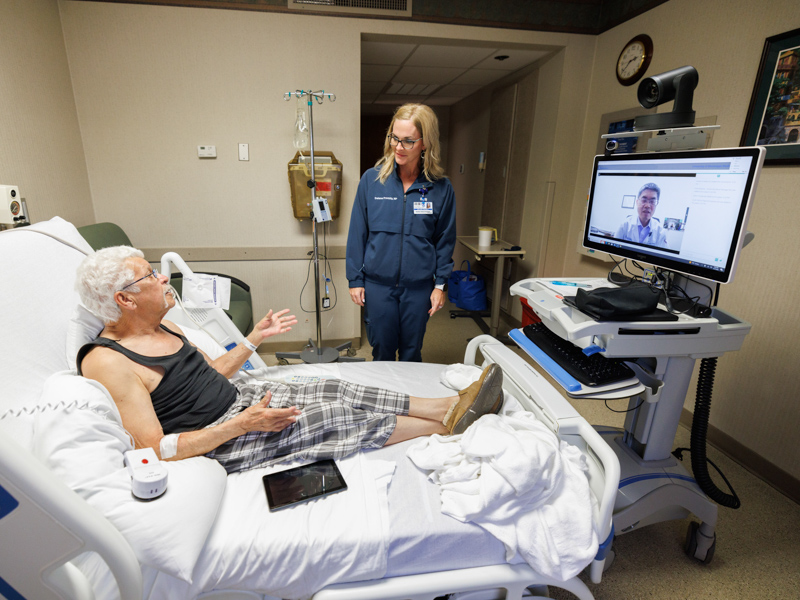
Huang was in his office at UMMC’s Translational Research Center in Jackson. Bustin was in his hospital bed in Laurel. But, they saw each other just inches apart during an audio-video visit facilitated by the UMMC Center for Telehealth.
The collaboration with SCRMC is noteworthy because it’s the first time UMMC has provided specialty care for hospitalized patients via telehealth, not just those visiting a clinic or an emergency room, said Dr. Alissa Willis, associate professor and chair of the Department of Neurology.

“I don’t know of anyone throughout the state using this model for neurology care,” she said. “We are providing a full neurological evaluation customized to what’s going on with that patient, that day, keeping their care in the community and closer to home.”
The opportunity evolved after the retirement of one of SCRMC’s two neurologists. SCRMC asked UMMC to offer remote neurological evaluations and care to fill the gap.
“The working relationship between SCRMC and UMMC is a great benefit to our patients and our community,” said Doug Higginbotham, president and chief executive officer of SCRMC. “By offering these services to patients in Laurel, we are able to keep patients in their local community and they will still receive quality neurological care.”
“We’re providing something that the community really needs,” said Dr. Shreyas Gangadhara, chair of clinical operations in the Department of Neurology and director of teleneurology inpatient services at SCRMC.
“We ramped up our services so that we could provide inpatient rounding coverage as well as 24/7 emergency consultations when needed,” Gangadhara said.
For two weeks of the month, SCRMC neurology nurse practitioner Delane Pressly and her colleagues spend their afternoons rolling a telehealth cart to patients needing neurology care, be that on a regular floor or in the intensive care unit.
She facilitates the live audio-video visit between the patient and a UMMC neurologist who examines the patient, reviews their vital signs and has a conversation with the patient and Pressly.
During the March 27 visit with Bustin, Huang led his patient through neurological testing. “I don’t want to stand on my head and stack BBs,” Bustin joked when Huang asked him to stick out his tongue and move it from side to side.
“Give me a big smile,” Huang said. “Now, close your eyes and open them. Move them to the left. The right. Look up. Look down toward your feet.”
Huang asked Pressly to gently touch Bustin’s hands and arms. “Can you feel this?” she asked Bustin. “Does it feel the same on both sides?”
“Oh, yes,” Bustin told her.
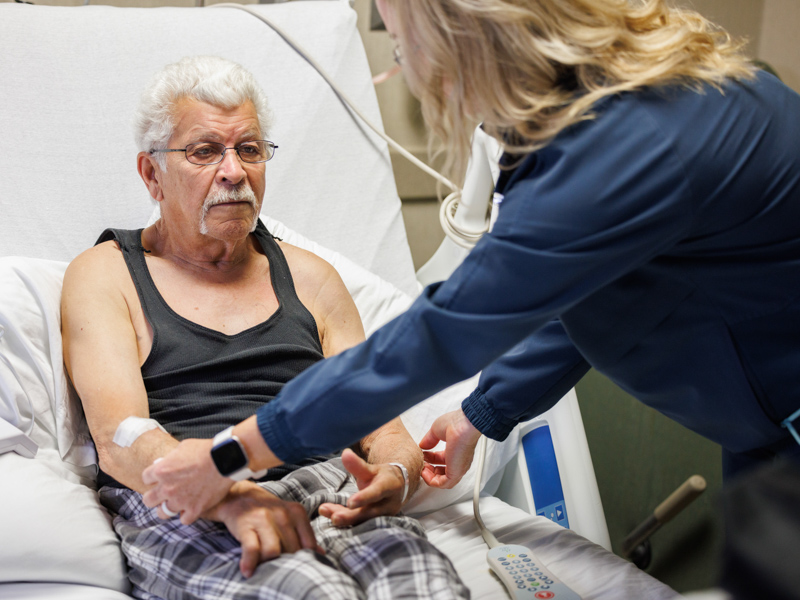
Then, Huang asked Bustin to get out of bed. Pressly stood near, ready to assist if Bustin needed help. “Take your time,” she told her patient.
“Put your feet together, and hold your arms in front of you. Close your eyes. Very good!” Huang said.
“We have full access to their medical records and imaging, and we go through their labs just as we would in person,” Gangadhara said.

“At the same time we are managing the patient, we can be communicating with their attending physician via a HIPAA-compliant messaging platform: ‘I saw your patient, and this is what I recommend.’ The doctor can reach out to us with questions,” said Dr. Saurabh Chandra, chief telehealth officer of UMMC’s Center for Telehealth.
“We communicate our care plan. We’re leveraging the technology that we have in order to do it all remotely,” Gangadhara said.
Although some community hospitals receive services from out-of-state telestroke providers, “our program isn’t limited to stroke, and we provide rounding to patients,” he said. “The others shift those patients to a larger hospital.”
“This teleneurology program is not a transaction where we are providing a one-time interpretation of what’s happening with the patient. We are helping to manage the patient as part of the team at SCRMC,” Willis said.
“With severe shortages of specialists in the state, telehealth can bridge the gap in providing access to specialists for community hospitals, enabling them to manage the patients safely in their local communities,” Chandra said. “This is a win-win situation for everybody: patients, community hospitals as well as UMMC, as we can avoid unnecessary transfers to the only academic medical center in the state.
“The success of this project will allow us to implement similar programs with other specialties like critical care, cardiology, nephrology, etc.”
Common conditions treated also include seizures and altered mental status or confusion. “We treat everything and anything that is neurologically related,” Gangadhara said.
“When I talk to the patients and their family members, they’re so happy to see us and to get this care. We’re able to communicate and spend time with them on the screen, and we can call them afterward.”
Providers at SCRMC also are satisfied, Gangadhara said. “This is a win-win for the patients, the hospital and for us. We’re carrying out our mission to increase care in rural communities.”
“For a state with a population of approximately 3 million, there are only 60-70 neurologists total,” Willis said. “It takes a long time to recruit a neurologist to a small community, and it takes us eight or nine years to train a neurologist from medical school through residency.
“That makes what we are doing in teleneurology incredibly important,” Willis said. “Hopefully, this will evolve to serve more communities, and to connect medical students and residents to communities so that they’ll have a desire to stay in Mississippi and practice.”
Taking teleneurology to a rural community isn’t as easy as it might look. “A combined UMMC neurology and Center for Telehealth team worked with the hospital to make sure we had the technology resources on a tight timeline,” Willis said. “Dr. Gangadhara worked with me to rethink how we could quickly confirm coverage from our neurologists while still covering all UMMC services. He led training for UMMC neurologists and SCRMC’s nurse practitioners.”
If not for the Center for Telehealth IT team, Chandra said, getting the program up and running would have been more difficult. “We’ve learned a lot that will help us from a project management standpoint, and about the technology needed,” said Angie Haller, a Center for Telehealth project manager. “We’ve learned what equipment works best and what limitations WiFi has.”
Bustin is grateful to have local access to a neurologist, but hopes his next visit isn’t in the hospital.
“You’re ready to get out of here,” Pressly told him after Huang recommended a follow-up appointment. “I’m so glad you are better.”
“We certainly recognize that there are many other communities like Laurel that have lost some or all of their coverage,” Willis said. “We’d like to partner with other groups to provide neurological care close to home for those who need it.”


