Engineering the future of medicine

Published in News Stories on October 13, 2016
In Dr. Amol Janorkar's lab, the work is about better living through chemistry, biology, engineering and materials science.
Janorkar, an associate professor of biomedical materials science, studies tissue engineering. The goal is to use cells, materials and biologics to construct new ways to study and treat disease.
Tissue engineering is much more than the “ Vacanti mouse,” a rodent that made news headlines for the ear-shaped cartilage on its back. Rather, the goals are practical and noble: revitalizing livers, replacing cartilage and bone, and new skin for burn victims.
“That is the promise of tissue engineering… but solid organs, like livers and hearts, are farther down the road” and years from clinical use, Janorkar said. However, the basic science research is happening now in his lab at UMMC and at universities across the country.
One of Janorkar's projects, recently funded by a $1.4 million grant from the National Institutes of Health, takes on part of health care's largest challenge. He is developing and studying 3-dimensional models of human adipose tissue, or fat.
The model binds fat cells in a spheroid, or almost round, shape using elastin-like polypeptide and polyelectrolytes. A common protein, elastin is a component of mammalian fat tissue, making the engineered ELP a relevant tool to help hold the cells together, Janorkar said.
In a previous study, Janorkar “fed” the cells fatty acids to study how adipose grows and proliferates. On the current grant, he will add metabolic stressors like TNF-a to determine how they affect adipose development.
“By learning how cells become fatty, we can begin to answer the question, 'How can we make these cells lean again?'” he said.
These spheroids aren't visible to the naked eye, but Janorkar hopes they could become an important part of the drug development process.
“When drugs are first tested in vitro, scientists use 2-dimensional cell cultures,” Janorkar said. The cells grow as a single layer on a Petri dish. However, fat is not flat. Neither is any other part of the human body.
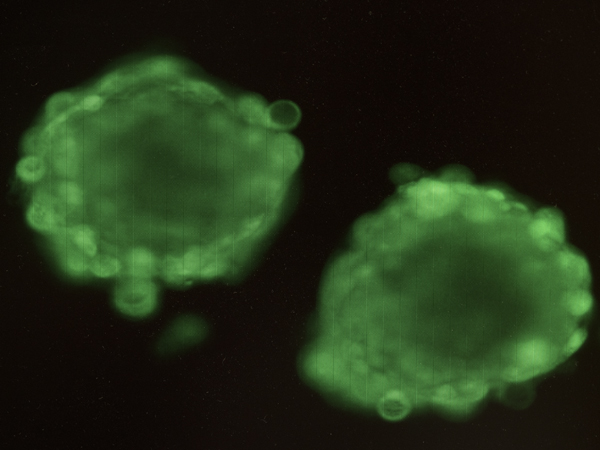
The 3-D adipose model under magnification. Charged polyelectrolytes and elastin-like polypeptide force fat cells together, forming spheroid rather than flat cell cultures.
As few as one out of every 5,000 drugs evaluated in laboratory tests makes it to clinical trials. A 2014 report in Nature Biotechnology found that only 10 percent of those receive FDA approval. Janorkar said this disconnect is one potential reason for the lack of approved obesity treatments and other pharmaceuticals.
In contrast to other in vitro models, Janorkar's 3-D adipose model is tethered by ELP above the culture plate like a balloon. The electric charge of the polyelectrolytes force the cells together, allowing them to interact with each other as they would in human tissue.
“If we can make more realistic in vitro 3-dimensional models, then we can potentially decrease the timeline and expense associated with drug development and make the system more efficient,” he said.
As part of the School of Dentistry, the Department of Biomedical Materials Science has a particular focus on applications for dental prosthetics and implants. Janorkar and two of his graduate students published research in the October 2016 issue of the journal Dental Materials testing composites for guided bone regeneration. GBR uses scaffolds and cells to regrow bone in patients.
In dentistry, GBR is used to “stabilize the foundation for the teeth,” said Dr. Matt Milner, assistant professor of care planning and restorative sciences.
“Think of the gums and bone as the foundation of a house,” he said. “If there is… a significant amount of erosion, then it is beneficial to stabilize the foundation and fill back in what was eroded [using] GBR procedures in order to save the tooth.”
Bhuvana Gurumurthy, a third-year Ph.D. student in biomedical materials science, is the paper's first author. She said the goal was to find composites with the most ideal mechanical properties, like stiffness and toughness, to withstand conditions in the mouth.
“The patient is going to be biting and chewing,” she said. “We want this implant to stay in the body for a long time.”

Bhuvana Gurumurthy, a third-year Ph.D. student, checks the cell cultures growing in the Janorkar lab.
In addition to durability, Gurumurthy said the ideal scaffold should biodegrade as bone regrows. Current GBR methods use scaffolds that require an additional surgery to remove. Therefore, the Janorkar lab made scaffolds with different amounts and ratios of ELP and collagen to make an ideal home for human adipose stem cells as they differentiate into bone.
In future studies, Gurumurthy plans to add bioglass and antibiotics to the composite and move forward the pre-clinical testing. As a dentist by training, she hopes her dissertation research will form a foundation for new clinical applications.
“If all of the properties of the scaffold work well, then there is a better opportunity for the materials to integrate into the body, and a shorter amount of time will be needed for bone regeneration,” she said.
Dr. Jennifer Bain, assistant professor and interim chair of periodontics and preventive sciences, said that clinicians look for additional properties in any GBR product.
“It needs to be easy to use. If [a GBR product] is too cumbersome to handle, then clinicians may not use it,” Bain said. “It also needs to be cost-effective,” particularly for patients who may pay out-of-pocket expenses.
Lastly, the regenerated bone needs support what is placed on top.
“It's all about the final result: the crown that goes on of the implant,” Bain said.
“It's like we are putting together a puzzle,” Janorkar said. “We want to build a composite that can do it all - help growth, fight infections, and limit the surgical procedures needed.”

The Janorkar lab, front row from left: Quynh Chau Nguyen, D2; Gurumurthy; Kendra Clark, D3; back row from left: Jared Cobb, Ph.D student; Sarah Fitzgerald, Ph.D. student; Janorkar.


