Education research: That’s their department
Just like the Milky Way, dinosaur bones and TikTok, learning how to teach can always use further study.
That is the thinking behind a newly-named department at the University of Mississippi Medical Center: the Department of Advanced Biomedical Education in the School of Medicine.
DABE, a re-organization of, and replacement for, the Department of Neurobiology and Anatomical Sciences, declared itself open for business as of July 1; its faculty will concentrate, not only on educating, but also on the best ways to educate.
That is: how to best explain material to students, how to show students the best ways to use this knowledge – and the best ways to remember it. It’s framing education as a research subject.

“This process is dynamic and evolving,” said the department’s leader, Dr. Norma Ojeda, professor and chair of the Department of Advanced Biomedical Education, “and the only way to keep up is adding innovation and research to the equation.”

While this idea is not new to the Medical Center, devoting an entire department to it is, said Dr. Loretta Jackson-Williams, professor of emergency medicine and vice dean for medical education. “This is not just about student education; it’s also about faculty development.
“In medical schools, there is a realization that a department focused on educational research and scholarship alone is needed,” she said. “We’ve never had such a department at the Medical Center.
“But some of the faculty are already doing that in a significant way: An example is the clinical anatomy program in the School of Graduate Studies in Health Sciences. It’s focused on developing faculty members who are adept at teaching that program; they earn a PhD.”

Now, they will still earn that degree in the graduate school but while working with the faculty who are in DABE, which offers what Dr. David Norris calls “a new home for faculty whose primary role is education.”
As they teach pre-clinical students – those in the early years of their education – faculty will be better able to explain to them exactly how they will one day, as professionals, move that mountain of classroom-acquired knowledge to the clinic, said Norris, professor of family medicine and assistant dean for academic affairs in the School of Medicine.
“Many of our faculty do a great job of this already. But, with this reorganization, a concept taught by one faculty member will be reinforced by others many times. It will all be in one course now.”

This departmental change underwent analysis and review for years before it was announced to the Medical Center at large, in May, by Dr. LouAnn Woodward, vice chancellor for health affairs and dean of the School of Medicine, who has described Ojeda as “an accomplished and skilled clinician-scientist and her dedication to medical training will set a tone for the new department. … ”
Much is still to be done, reorganization-wise, Ojeda said, and it will be August of next year before students, particularly first-year medical students, “will really see a difference.”
Still, departmental research will target the education program in general, and not just in the School of Medicine, Jackson-Williams said. Besides those in the medical school, faculty who teach in the schools of dentistry, graduate studies in the health sciences, and health related professions are among those who form what she calls “the inaugural group of the new department.”
All of the faculty in DABE are faculty within the School of Medicine, she said. “They are just each in other schools also.
“The department’s name reflects the full spectrum of the work done by faculty in many schools in biomedical science” – the combined study of biology and medicine to promote better health, with courses in anatomy, histology, epidemiology, physiology and much more.
As clinicians teach in these courses, Norris said, “we will bring to the surface all the baseline knowledge we use without even thinking about it. This approach will force us, as teachers, to slow down our clinical reasoning; then we can better explain to our students what we do: ‘This is how I arrived at this conclusion. This is how I decided to treat this condition.’”

Leading this charge is Ojeda, who is also vice-chair for research in the Department of Pediatrics. She has degrees, fellowships or certifications in everything from hematology to physiology, business to clinical investigation, internal medicine to medical education.
“She has the perfect background,” Norris said. “She is heavily involved in research. She is also a clinical professor and an excellent educator. The way she communicates with others is impressive.”
For her part, Ojeda is eager to chair a department that is, she said, “trying to become the biomedical hub for the next generation of health care professionals. “In addition, we are introducing state-of-the-art new technology to the learning process.”
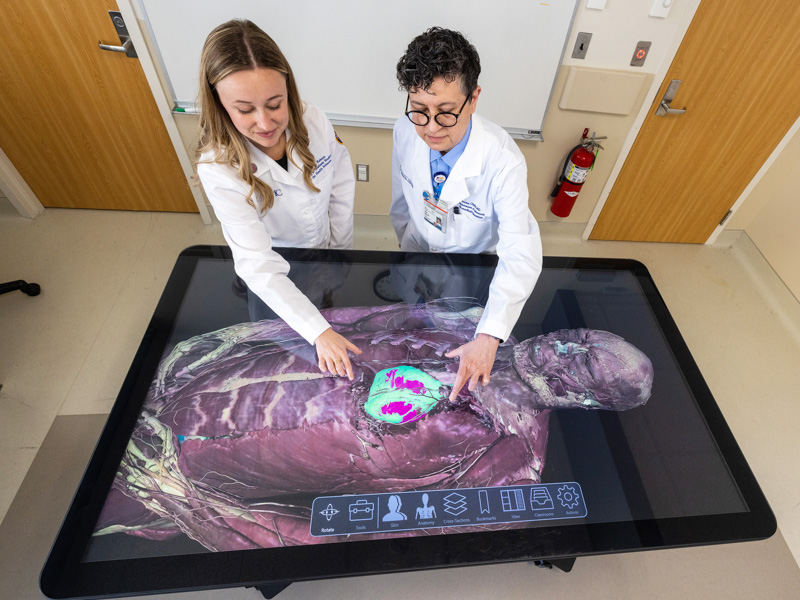
Students taking Gross Anatomy in the pre-clinical courses will be able to use a 3-D virtual cadaver and virtual dissection technology, she said. As for clinical students – those in the latter years of their training – they will use virtual simulation for performing procedures on virtual patients.
Students will “see their future selves,” Ojeda said. Practicing clinicians – specialists in family medicine, internal medicine, pediatrics, pulmonology, etc. – will bring their day-to-day experience with patients to the learners who, pre-DABE, would not have enjoyed this kind of practical learning until later in their training.
These pre-clinical students will learn, for instance, not only where the lungs are, and “why you have two of them,” Ojeda said, “but also how the shapes of the structures in the thorax support and protect them, and conditions affecting them.
“This makes it much easier for the students to connect the dots, and this connection is critical for them. But the teachers will also learn from the learners: How to best deliver the information they are trying to impart. It’s two-way learning.”
Much of the learning will happen in an academic orbit with a name that sounds like a job for NASA: ISTARS, or Interprofessional Simulation, Training, Assessment Research and Safety.
ISTARS embraces several programs or venues: the Simulation and Interprofessional Education Center, Basic and Advanced Resuscitation Training Center, and Judith Gore Gearhart Clinical Skills Center.
This is one of the major differences between DABE and its predecessor: The latter did not include these centers. Because DABE does, it will be easier to reach a “standardized level of training for all our health care professionals,” Ojeda said.
There will be more opportunities for the much-desired aim of interprofessional education – placing in one setting students from different schools so they can learn together – and from each other.
“We can create new scenarios within the Simulation Center; for example, the proper way to gown during encounters with patients during a pandemic,” Ojeda said. “How to protect them, but learning how in a safe environment.
“These educators and trainers in DABE and ISTARS are the top, top in their field. I am so honored to be working with them and taking biomedical education to the next level of excellence.
“I am so glad to be in this department.”
Department of Advanced Biomedical Education goals:
- Provide a primary academic home for select faculty who represent various disciplines, but whose primary role is teaching;
- Strengthen the horizontal and vertical integration of curriculum content and delivery of the educational program;
- Promote scholarly work and improve the quality of research in areas with an educational focus;
- Promote and support interprofessional education;
- Support faculty development for master educators;
- Provide appropriate administrative support for the delivery of the educational program; and
- Manage all auxiliary services that are integral to the educational programs.


