Masks foil lipreading for those with hearing loss; you can help
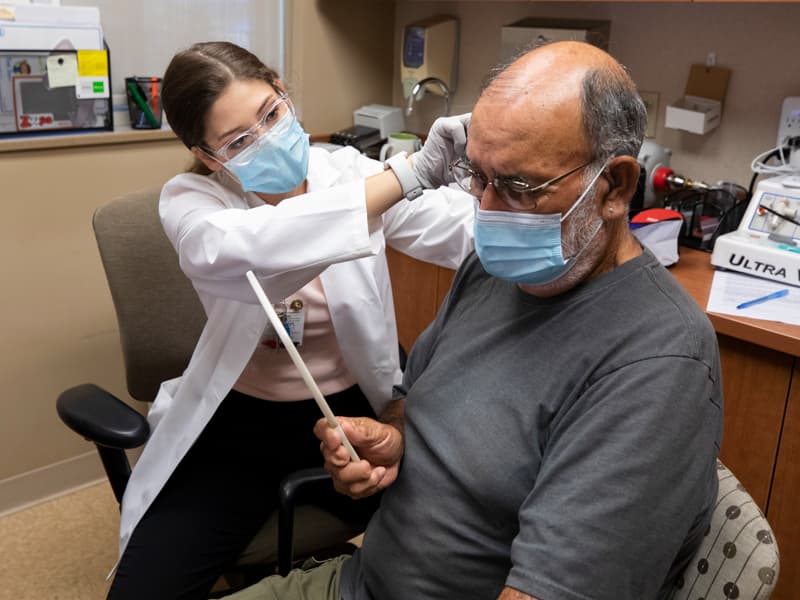
If wearing a mask is helping slow the transmission of COVID-19, it’s also suppressing the spread of something basic to reliable health care: good old-fashioned give-and-take.
This is decidedly true for patients who depend on lip-reading to understand what their providers are saying.
Of course, when lips are masked, the ability to read them is lost, and, minus remedial measures, something is lost in the translation.
But there are remedies health care workers can take – not just for the hearing impaired, but for all patients when facial coverings are required; in fact, almost anyone can use some of these approaches in everyday, COVID-warped conversation.

“All of us, even when we don’t have a hearing loss, utilize a lot of cues when someone is talking, whether we realize it or not,” said Dr. Catherine Sassano, assistant professor in the Department of Otolaryngology-Head and Neck Surgery at the University of Mississippi Medical Center.
“We have a lot of strategies we can use when hard-of-hearing patients can’t see our lips.”
Speaking louder, however, is not always one of them, said Lauren Langan, an audiology extern and doctoral candidate who works with Sassano.

“I have a hearing loss myself,” Langan said, “and when someone talks louder to me, they can sound frustrated. When hearing-impaired patients notice that frustration, it’s hard for them to ask for repetition, because they don’t want to be a burden.”
Lorenzo Valdez, 74, of Pelahatchie has sensed aggravation in the voices of people in phone conversations, where certain, subtle sounds are difficult to make out.
“I just try to let [the aggravation] roll off me,” said Valdez, whom Sassano recently fitted for a new hearing aid. “But one time, I did tell someone, ‘One of these days you’re going to be my age and you’ll find out what it’s like to be hard-of-hearing.’”
Often it’s like this: People just start talking louder. But that may not help, Langan said, particularly with a type of hearing loss common in older adults.
“Loudness can cause distortion. So, instead of talking louder, talk more clearly.”
And rephrase questions, Sassano said. “If you ask a patient, ‘What did you do this weekend?’ and they ask for repetition, say something like: ‘Did you spend time outside with your family this weekend?’
“That way you’ve added information.”
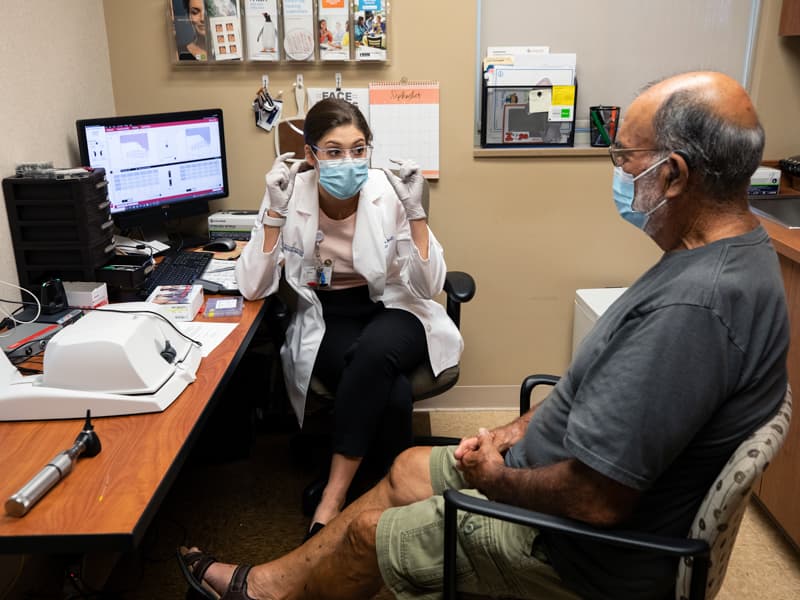
To be transparent, so to speak, audiologists and others do have a not-so-secret weapon: clear masks, which allow patients to read their lips.
“But when we see patients in the ENT clinic for only about 25 or 30 minutes, there’s not much time left for counseling in this fast-paced setting. So we wear surgical masks. We don’t use these communicator masks, unless it’s for hour-long appointments – and only if the patient continues to struggle to communicate,” Sassano said.
“We love to place the emphasis on listening.” The clear masks are for backup.
“When we don’t wear the clear masks, we make sure to talk more slowly; we are enunciating, especially the t’s, the ch’s and other consonants that also carry the meaning of speech,” she said. In other words, those sounds masks tend to swallow up.
You also have to make sure the patients are really hearing you, though, Langan said. “You don’t want to go through an entire case history and counseling, and they haven’t understood everything you’ve said.
“If I see patients just nodding while I’m talking to them, that is when I will ask if they can hear me OK. If they aren’t giving any kind of feedback, there is no way to really know if they’re actually understanding you. Verbal confirmation is almost always better.”
Go a step further, Sassano said, and ask if there is something else you can do to make yourself heard.
But know that not every one of these steps will work in every case, she said. “When we’re not wearing clear masks, we often have multiple masks, including N95 respirator masks. “For patients with severe or profound hearing loss, rephrasing and greater volume won’t help.
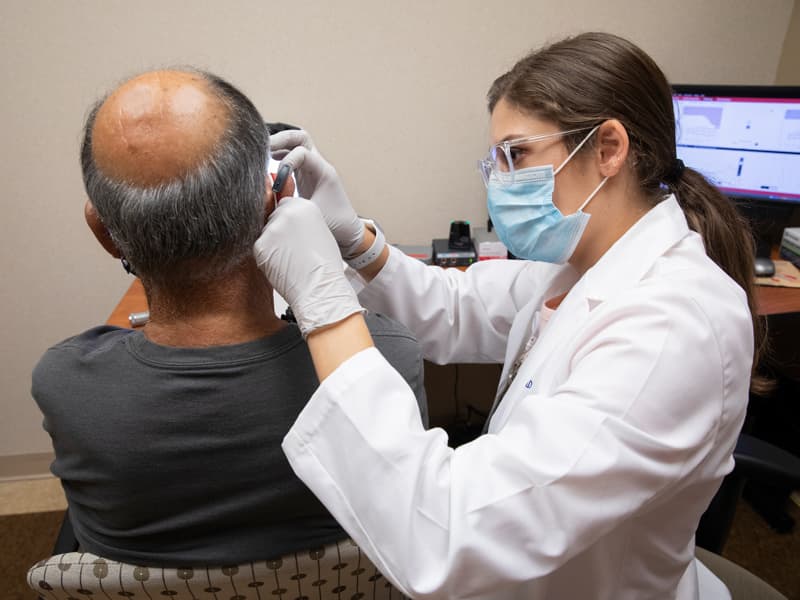
“That’s when you want to consider something else.” That includes the “talk-to-text” smartphone feature. “I open up the Notes section on my cell phone,” Sassano said, “speak into my phone and then flip it to patients so they can read what I’ve said.
“Audiologists have some patients who may need cochlear implants, patients for whom a hearing aid is inadequate. So when I see anyone to determine if they are implant candidates, I might have to use texting.”
Or she may use the Microsoft Word app to type out her messages and questions, she said.
Still, Sassano and Langan are more likely to see patients who can benefit from hearing aids. Valdez is one of them. Almost as soon as he was fitted for his new aid, he noticed a difference of “100 percent,” he said.
“People had been telling me to turn the TV down at home. I could see the picture, but I couldn’t understand half the words they were saying. I think this will help. Driving [back from his fitting] in the car, I had a conversation with my daughter and she didn’t have to yell. Until then, I never heard the air conditioner in my car.
“I’m going to have get used to hearing again.”
That’s a problem a lot of people would like to have. Untreated, even a mild hearing loss can hamstring comprehension, Langan said, “especially when there’s a lot of background noise: the TV playing, water running, dishes clanking.”
Eliminating those sounds in the home can keep aggravation at bay, she said.
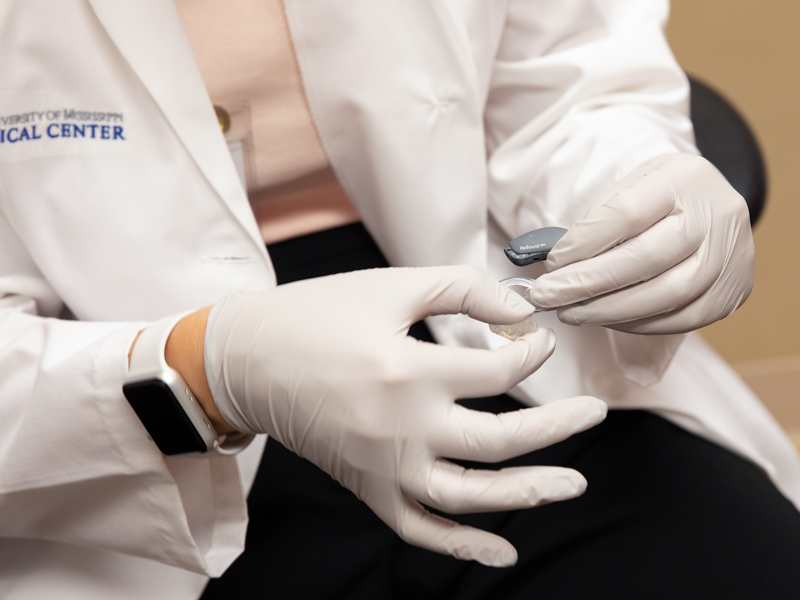
Even when patients have hearing aids, such steps are helpful, Sassano said. “They are called hearing ‘aids’ for a reason. They are not a hearing cure. When you put on eyeglasses, the lens corrects the impairment.” But, with a hearing loss, “you are working with a damaged system.”
So, expectations must be realistic. When pots and pans are clinking in the sink, a patient may not be able to hear a loved one across the house.
“So we tell the spouse or partner, ‘Get closer, face her, make sure there’s good lighting, minimize background noise.’ This is what we recommend when they are at home not wearing masks,” Sassano.
Despite the inconveniences of covering up, patients are, mostly, masking up willingly, said Skye Stoker, director of the Office of Patient Experience at UMMC.

“We have seen very little reluctance to wear a mask among them. The only feedback we’ve had from them about masks is when someone on staff isn’t wearing one. They are holding us accountable.”
Even so, in patient-provider encounters, it’s hard to make a full connection with only half a face.
“We’ve talked about this barrier: ‘How can patients read empathy on your face when they can’t see all of it?” Stoker said.
Maybe they can’t; but they can read your coverings. At UMMC, some caregivers have put their names on their masks to make them more personalized and inviting.
“Staffers in radiology oncology have laminated large photos of themselves and applied them to their uniforms; they’re much larger than the photos on the ID badges,” said Hillary Basden, manager of the patient experience programs.
All this helps patients and caregivers relate, Stoker said.
This is particularly important for those who are hearing impaired. At UMMC, those patients may avail themselves of American Sign Language interpreters, 24-7.
For those who can’t read sign language, there are language service tools, including the Stratus video interpreting device, which propel patient/provider dialogue.
“Our patients have that interpretive support even when wearing masks,” Stoker said. “We’re striving to connect and communicate effectively with them, even with our mouth guarded, and I think we’re doing a good job.”
While most Americans are looking forward to the day when we no longer look like we’re about to hold up a liquor store, Sassano would like to “shine a light” on one convenient consequence: The ears of the hard-of-hearing are being forced to “stretch their legs,” she said.
When they’re communicating with someone wearing a face mask, “they can’t rely as heavily on their ability to lip read to compensate for the fact that their auditory system is adjusting to a novel way of hearing.”
With a 30-minute grocery store errand, for instance, they have to practice active listening and conversational back-and-forth.
Although unintentional, Sassano said, “that would be comparable to a 30-minute session of aural rehabilitation.”
In this Golden Age of Masks, there’s at least one silver lining.


