UMMC surgeon now offers micrographic surgery for early stage melanoma
Using Mohs surgery to remove melanoma in situ can leave less scarring and fewer visible reminders of this deadly skin cancer.
Dr. William Black, an associate professor of dermatology and a Mohs surgeon at the University of Mississippi Medical Center, is one of only a few Mohs surgeons nationwide who uses the technique to remove these early stage melanomas.

Black said the technique is usually used on melanomas on a person’s head and neck, hands and genitals.
Several Mississippi dermatologists use Mohs on non-melanoma skin cancers such as basal and squamous cell carcinoma. The UMMC Cancer Institute’s skin cancer team offers Mohs surgery for melanoma and non-melanoma cancers.
Mohs surgeons use special equipment to remove thin layers of skin, then look at the layers under a microscope to be sure the margins, or edges, are clear of cancer. If not, the surgeons can remove more layers to get all of the cancer. Additional surgical and pathology equipment is needed to do the same surgery for melanomas.
“The main idea is, you are checking for margins,” Black said. “With the standard way of excising things, you’re actually checking a small percent of the margin for cancer. With Mohs, doctors are looking at the complete margin. Because you’re looking at 100 percent of the margin, you can cut a smaller amount of tissue, which generally leaves a smaller scar.
“If you have a positive margin, in real time, you see that. You’re not bringing these patients back another day to remove more cancer.”
The Mohs surgical team removes the skin, prepares it, stains it with chemicals so malignant cells are highlighted, looks for malignant cells and seeks margins that have only normal cells. If the margins show malignant cells, the team removes another layer of tissue and repeats the process.
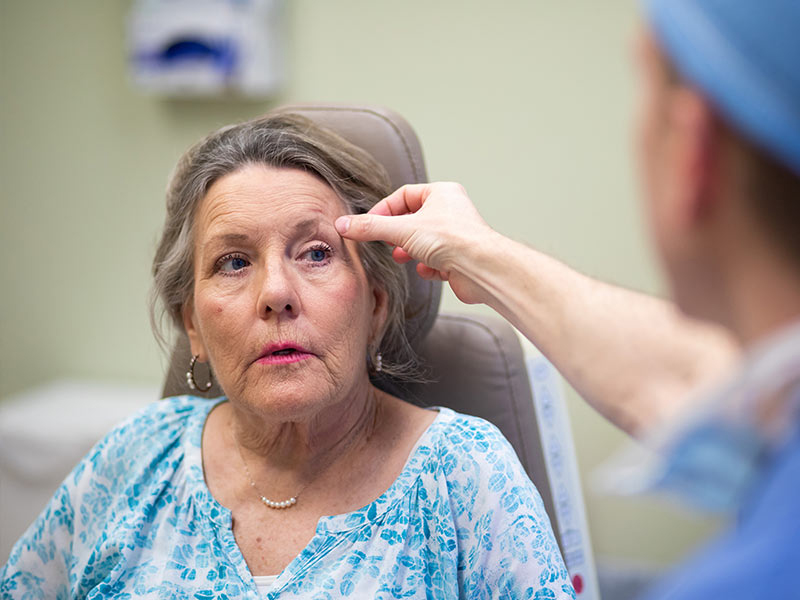
Linda Puckett of Ludlow had Mohs surgery for a small melanoma on her forehead. Her dermatologist, who does not offer Mohs, referred her to Black.
“It was flat, not noticeable,” Puckett said. “This was in my eyebrow, about the size of a dime. It had been there for years.”
Black said Puckett’s story is not uncommon.
“It looked like a sun spot,” Black said.
Catching it early before it exhibited traditional signs of a cancer was fortunate. It’s unlikely it was always malignant, but doctors have no way to determine when it became a melanoma. Puckett was a good candidate for Mohs surgery, Black said.
Puckett said she’s pleased with the results and shows photos of the early stitches and continued healing. Today, a faint scar and a bit of puckered tissue under the eyebrow are all that remain. Black said those are likely to fade further; If they don’t, another short procedure can help.
The hardest part was waiting, Puckett said: The entire procedure took about five hours.
“That was the only unpleasant thing, and knowing I had this gaping hole in my head,” she said.
Black had removed skin about the diameter of a 50-cent piece, she said. Puckett had to remain seated with the wound covered while Black looked at the slides. Then doctors sutured the wound.
More than six months later, Puckett said it’s healed.
“People that know I’ve had that done say, ‘I can’t even see a scar,’” she said.
Her medical follow-up procedure includes doctor visits every six months for the next three years to be sure no more melanomas appear.
Tips to lessen risks of skin cancers:
• Wear broad-brimmed hats.
• Stay in the shade from 10 a.m.-2 p.m. when ultraviolent rays are strongest.
• Wear sunscreens with sun protection factors of SPF 30 or higher, also labeled broad spectrum UVA-UVB blockers.
• Reapply sunscreens every two to three hours, especially if swimming or sweating.
• Wear sunglasses with UV protection.
• Check for new growths, changing moles or sores that will not heal on the body on the first day of every month. Find a partner to check the back.
• Show suspicious spots to primary care physicians or dermatologists.



