Boater’s accident demonstrates why UMMC is ‘Ground Zero’ for emergencies
Minutes after her husband Dan was viciously sliced by the propeller of his boat on Lake Caroline, Ann Smith wrapped her arms around him and prayed that it wouldn’t be his time.
Fortunately, it wasn’t.
“So many miracles,” she said of Dan’s journey of healing that began with his early afternoon accident April 24, 2017, on the neighborhood lake in Madison County.
Her prayers weren’t just answered at one of the docks where Dan fell out of his new boat after a wake unexpectedly jostled it. They also were answered at one of the University of Mississippi Medical Center’s four adult intensive care units, and before that, in the hospital’s Emergency Department.
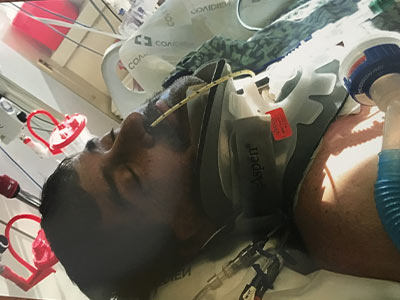
“They didn’t care who he was or whether he had insurance or not,” Ann said. “They didn’t even ask his name. They took him straight to surgery.”
UMMC is the state’s only Level I trauma center, a designation awarded by the Mississippi State Department of Health. The Medical Center offers advanced services, equipment and expertise to patients who have suffered traumatic injuries that aren’t available at other facilities in Mississippi. The health department has designated those facilities at Levels II-IV.
Traumatically injured children and adults usually arrive by ambulance or in UMMC’s AirCare, the state’s most advanced medical helicopter transport.
“We often get referred from other facilities the injuries that are complex or require subspecialty care,” said Dr. Alan Jones, professor and chair of emergency medicine. “We treat over 70,000 adult patients annually, the highest emergency department volume in the state.”
As a Level I trauma center, UMMC has a combination of physicians, surgeons and residents in subspecialty areas at the hospital 24 hours a day, seven days a week.
“At a Level II hospital, they have to call in a trauma surgeon from home,” Jones said. “They don’t necessarily have orthopaedic surgeons or neurosurgeons.”

In Dan Smith’s case, a complete trauma team swiftly reported to his operating room. Among them were Dr. Matthew Kutcher, trauma surgeon; Dr. Benjamin McIntyre, plastic surgeon; Dr. Pierre de Delva, thoracic surgeon; Dr. Randall Jordan, ENT physician; Dr. Laura House, ENT resident; Dr. Wade Christopher, surgery resident; and Dr. Hess Robertson, anesthesiologist and critical care physician.
“He had broken all of his ribs on the left side,” Kutcher said. “You could see where the propeller hit him. His vital signs were OK, but he had a bad critical care problem in that his left lung was not functioning. The force it took to break the bones was transmitted to his lungs.”
Thus began the Madison resident’s four-plus-week stay in the Medical Center’s Surgical Intensive Care Unit.
“Hold tight”
The Smiths had their two granddaughters that day on the lake.
“Dan was off and we were going to take them out on the boat,” Ann said.
Their boat was new, so Dan was being extra careful. But he hadn’t turned on the boat’s kill switch, which attaches to the driver’s belt and shuts off the engine if the driver falls out.
Before the girls had a chance to board, the wake caused Dan to roll out of the boat.
“The motor propeller got his jaw and his lung,” Ann said. “He was under water and I didn’t know where he was.”
Ann ran to the lake’s clubhouse for help, then headed back to the boat and saw her husband.
“He said, ‘I have lost a lot of blood. Look at this.’ He was talking about his chest. He said, ‘I’m weak.’
“I laid down on the pier and said, ‘I love you. Hold tight.’ Then he got his arms wrapped around my neck.”
“I remember standing up in the shallow water, looking at my chest and thinking, ‘Lord, I guess this is it for me,’” Dan said. “Apparently, I was able to get to the pier, even though I don’t have a recollection. I can only answer that Jesus carried me.

“From that time until about a month later, I have no memory.”
Help began to arrive. First responders and an ambulance rushed to the pier. A woman came from across the street to watch the grandchildren. A man turned off the boat’s engine.
“Oh, my goodness. They were wonderful,” Ann said. “There were people all over, praying for Dan.”
The first responders wasted no time summoning AirCare.
“I remembered that UMMC was trauma care,” Ann said. “I remember saying to one of the first responders that they always carry you to the nearest hospital and I asked where he (Dan) would be carried. They said UMMC. I said, ‘Great!’
“I knew he was bad, but I didn’t realize just how bad.”
AirCare left the Medical Center bound for Lake Caroline at 1:50 p.m., arrived at 2 p.m., then left with Dan at 2:18 p.m. before arriving at UMMC at 2:26 p.m., according to Stephen Houck, a former AirCare paramedic who manages Mississippi Med-Com, the statewide emergency communications system located at UMMC. AirCare has four helicopters, all staffed at minimum by a pilot, registered nurse and critical care paramedic.
“You’ve done all of your treatment en route that you can do,” Houck said. That can include procedures that only AirCare is qualified to do in the state, such as the insertion of chest tubes; the administration of Kcentra, a medicine that can stop profuse bleeding in certain patients by reversing anticoagulants; or the placement of arterial lines to monitor blood pressure by the second.
In the trauma room, “they want to know right then what happened,” Houck said. “You get about two minutes to give your report and then they hammer you with questions. ‘What happened?’ ‘What did you see?’ ‘What did you do?’ ‘What do you think might be going on?’
“It can be overwhelming, but we’re not overwhelmed. Everyone brings the worst of the worst here. That’s what makes our trauma center so unique.”
Critical care and prayer
With no family yet at his side, Dan temporarily became “Unknown Aqua.” ED staff assign colors to patients who can’t immediately be identified.
Kutcher said when a traumatically injured person arrives at a Level I trauma center, saving them is “not necessarily getting the right surgeon. It’s going to the place with the right resources.”
That includes a trauma team to compliment the trauma surgeon, who is “trained to take care of a little bit of everything,” Kutcher said. “We are experts in stopping potentially fatal bleeding and resuscitating patients who are critically ill.”

Within minutes of Dan’s arrival, Kutcher said the patient had a CT scan to assess the extent of his injuries. Just a few minutes later, trauma surgeons and other medical specialists, including plastic and thoracic surgeons, were in place in the OR.
“It’s not a situation you have at many hospitals,” Kutcher said.
The next day in the surgical ICU, Dr. Leon Sykes, trauma and critical care physician, explained to Dan’s family why Dan needed not one, but two vents to breathe.
“He had a hole in his left lung and the air was escaping,” Ann said. “He needed one vent to keep the left lung from collapsing and one to keep the right lung going.”
That night, the medical team called a family conference, explaining that Dan’s condition was dire. Even so, Ann said, “I had a really strong peace that he would live.
“On Thursday, they allowed our ministers and elders to come in. They laid hands, prayed and anointed him with oil.”
Dan’s family wondered if the impending wedding of his daughter, Sarah Smith Boyd, might need to take place in the ICU.
Ann said the family bonded with the nursing staff, the residents, “even the security people in the waiting room. We could not have asked for better hospitality and caring,” especially from Kimberly Horn, Scott Hallman and Rachael Banks, nurses, and Christy Barrick, nurse practitioner.
And there were the miracles.
“When doctors said the only thing left to save him was the ECMO machine, we prayed and his lungs got a little better,” Sarah said. “When doctors said he would go on dialysis, we prayed and his kidneys started working.
“When doctors said his left lung would be removed, we prayed and a blood clot disappeared and his lung started working again. When people feared he was too weak for rehab, we prayed and he walked 50 feet the first day.”
“From reviewing records and hearing from my family and doctors, I realize how blessed I am to have survived,” Dan said.
He was discharged from UMMC in early June 2017 to continue therapy. On June 10, 2017. Methodist Rehabilitation Center approved him to leave briefly to “walker” Sarah down the aisle.

“I not only survived but I was able to participate in the wedding less than seven weeks after the accident, including a dance with my daughter,” Dan said.
A year later, he continues to recover. His caregivers also include Dr. Ron Caloss, associate professor of oral and maxillofacial surgery in the School of Dentistry, who performed the first of several jaw reconstruction surgeries on May 7, 2018.
“The Lord has placed us with the best of the best,” Ann said.
Dan has several messages to convey.
“If you are a boater, please take all safety measures seriously,” he said. “If I had been wearing the kill switch, this probably wouldn’t have been a story. Support UMC when possible. They are excellent. Be thankful for every day. Most of us don’t really have bad days.
“If you don’t believe in miracles, I would like to have a conversation.”



