UMMC's 'ambitious' pain relief program protects patients from addiction
A team of University of Mississippi Medical Center physicians and caregivers is changing the way they offer patients pain relief at a time when an average half-million opioid pills are dispensed daily by doctors statewide.
The Medical Center’s pain management physicians are partnering with the UMMC Department of Psychiatry to develop a first-time clinical treatment model addressing the issue of opioid abuse. The goals are to effectively manage and minimize patients’ pain and give them quality of life and improved function by starting them out, not with opioids, but with other medications or non-medicinal remedies that can protect them from addiction.
It’s an ambitious program that impacts not just people at home with chronic conditions, but hospitalized patients who may have just been wheeled away from the operating room.
“The mindset change of using opioids only as a rescue drug is already in place,” said Dr. Ken Oswalt, UMMC assistant professor of anesthesiology and leader of the Medical Center’s acute pain service. “We are limiting use of opioids in the hospital now.”

Dr. Douglas Bacon, professor and chair of anesthesiology at UMMC, and his staff are spearheading the effort to build and implement the treatment model with assistance from the Department of Psychiatry, led by Dr. Scott Rodgers, professor and chair of psychiatry. Development of the model has the backing of UMMC’s top leaders.
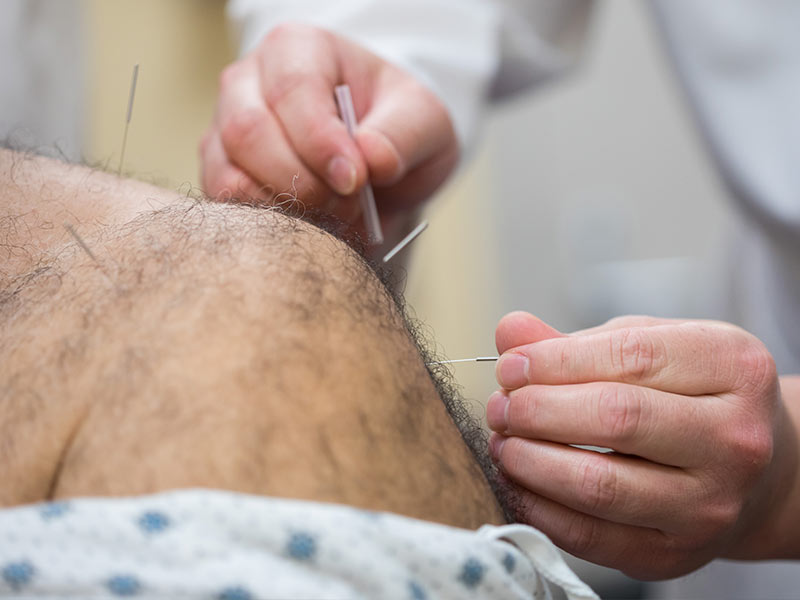
“We’re looking at acupuncture and other non-medicines, such as physical therapy and occupational therapy,” said Dr. William Gusa, UMMC assistant professor of anesthesiology and the Medical Center’s vice chair for pain services. “There’s not a structure right now to incorporate that.”
Plain and simple, Bacon said, doctors – as a community - “prescribe way too much opioids.”
The work at UMMC comes as the state Board of Medical Licensure is proposing an overhaul of regulations to the prescribing of opioid drugs, a policy shift that has attracted both criticism and praise. Twenty-four states have passed laws limiting opioid prescriptions, but Mississippi isn’t one of them.
The board’s proposed changes would mandate that physicians prescribe the lowest effective dose of opioids for acute pain and not more than a 10-day supply. The policy also would discourage physicians from prescribing more than a three-day supply of opioids and would allow an additional 10 days if clinically necessary, but with a new prescription and documentation of why the prescription is necessary.
The proposed changes also would include a requirement that providers run the name of each patient receiving an opioid prescription through the state’s online prescription monitoring program to check whether the patient has already received prescriptions from other providers. That regulation would apply to any patients coping with acute or chronic non-cancerous and non-terminal pain.
And the proposals include a requirement that patients be drug-tested each time they receive a Schedule II narcotic for chronic non-cancer, non-terminal pain. At a minimum, patients would be tested for opioids, benzodiazepines, amphetamines, cocaine and cannabis.
“That’s a big change,” Oswalt said. “The current thinking is to decrease the adverse effects of opiates. How do we do that and provide good pain relief?”

Physicians also have a responsibility to treat those who are addicted, Rodgers said.
“We’re talking about pain management and addiction, but there hasn’t been a formalized program to manage addiction at UMMC,” Rodgers said. Under development is a 40-hour-a-week outpatient clinic for substance abuse treatment, plus designating some Medical Center inpatient psychiatry beds to those sick enough to warrant hospitalization.
“You need counselors, social workers and psychologists” on the health care team, Rodgers said. “The notion of 90-day rehabilitation care is just not true. There’s a very high relapse rate. What works is outpatient services, and it has a much lower relapse rate.”
The goal is to prescribe opiates as a last resort when other remedies don’t work. Cancer patients, however, are not part of that discussion.
“Cancer legitimizes the pain issue. Non-cancer pain does not,” Oswalt said.
Here’s what UMMC pain management providers are doing as they fine-tune a new treatment model and change the Medical Center’s culture of pain management:
They’re treating pain with non-pharmaceuticals. Examples include acupuncture; behavioral therapy and counseling; physical therapy and occupational therapy; plus patient education.
They’re giving patients non-opiate medications such as acetaminophen, ibuprofen, aspirin; muscle relaxers such as Baclofen; local anesthetics and naproxen. When appropriate, some patients are treated for pain with anticonvulsants such as Lyrica or Neurontin, or with selected antidepressants such as Cymbalta or Pamelor.
They’re focusing not just on proper anesthesia and pain treatment during surgical procedures, but on a patient’s post-surgery pain through what’s known as Enhanced Recovery After Surgery. It calls for a multidisciplinary team of providers to adopt a culture of reducing a patient’s stress response to surgery as a way to help the patient recover more quickly.
“Part of this is having realistic expectations on pain,” Gusa said. “Patients should expect pain after surgery.”
They’re getting on the same page with fellow providers across the Medical Center, from family medicine to surgery to UMMC’s smoking cessation program. “There’s good collaboration between departments,” Rodgers said. “There’s a togetherness around this issue.”
They’re encouraging patients to take advantage of the Medical Center’s new Center for Integrative Medicine. Its caregivers work with chronic pain patients on lifestyle modifications related to diet, exercise, vitamins and physical therapy, said Stacey Kitchens, a psychiatric mental health nurse practitioner and the center’s associate director.
In the School of Medicine, physicians will teach students how to manage pain as a key part of their education. “We’re bringing together clinicians and scientists to come up with a curriculum on pain management and assessment, pain expectations and psychology,” Oswalt said.
UMMC’s Pain Management Center offers services for acute pain that include epidural analgesia, nerve blocks, local anesthetics and anti-inflammatory drugs in addition to opioids. Staff also work with patients using biofeedback, a non-drug method of self-regulating behavior to manage acute and chronic pain, especially in headache or migraine sufferers. Patients learn to control breathing and heart rate and to take steps to ward off looming pain with relaxation or stress management in addition to medication.
Caregivers in the Department of Psychiatry do not directly treat or prescribe medications to patients for their pain, but have conversations about addiction.

According to Dr. Mark Ladner, UMMC associate professor of psychiatry, when patients come to the outpatient psychiatry department, the prescription monitoring program is reviewed “to see if there are any patterns consistent with abuse of medication and addiction. Many patients may be embarrassed to start a conversation about addiction, and this is one way to start a conversation.”
Patients with stressful life issues can have more difficulty dealing with addiction and with coping with the changes needed to taper off opioids, Ladner said. These patients’ perception of pain can be impacted by their psychological state of mind and problems such as depression and anxiety, he said.
“We can treat the depression and anxiety, and this may improve the patient’s ability to cope with pain,” Ladner said.
Bacon said he wants to educate physicians who are discharging surgery patients from the hospital on the appropriate amount, strength and duration of opioids they’ll need at home.
“Seven percent of surgical patients who have never been on a narcotic before then will be on it 12 months after surgery,” Bacon said. “That’s a staggering number.”
According to Oswalt, physicians need to do a better job of explaining to some patients that they might never be totally pain free, but that a ready bottle of opioids will do them no favors in the long run.
Realistically, “you can be pain-free and dead, or you can have pain and be breathing,” he said.



