Geriatrician gap threatens crisis for the aged

Published on March 30, 2017
NOTE: This article originally appeared in the Winter 2017 issue of Mississippi Medicine, the semi-annual alumni magazine for the School of Medicine.

Dr. Mark Meeks knows there aren't enough doctors like him, because there are too many patients like his - geriatric patients dealing with pressure ulcers, incontinence, osteoporosis, limited mobility, Alzheimer's disease.
The number and scope of these cases is only going to grow, the byproduct of a population whose age is showing, said Meeks, professor of medicine and director of the UMMC Division of Geriatrics.
In Mississippi alone, within this group, well over 100,000 have been labeled “vulnerable.”
By one estimate, the state could use a geriatrician for every 700 of these adults - usually defined as those 65 and older. It has one for every 5,000.
“There will never be enough geriatricians in the country or the state,” Meeks said, “unless something dramatically changes.”
‘NO ONE RALLIES FOR US’
“People are living longer,” said Sharlene McLemore, who's in her 80s, a patient of Meeks' who resides in a Madison retirement community, St. Catherine's Village.
“We're blowing away the actuarial tables, particularly here at St. Catherine's; we're well cared for and have the kind of socialization others our age many not have.”
Often, people that age can use a physician who has been trained in skills medical students and residents rarely encounter, as a rule. Considering the magnitude of the approaching wave, this may sound untenable.
Nationwide, there are about 44 million older adults, but that number will swell to 71 million by 2029, the U.S. Census Bureau estimates. This influx has been labeled the “silver tsunami.”

Sharlene McLemore, 82, of Madison, one of Dr. Mark Meeks' patients, says geriatricians are more likely to be familiar with the needs of people her age.
“So we need doctors who are familiar with what happens to us, mentally, physically, emotionally,” McLemore said. “When I heard about Dr. Meeks, I said, 'That's the kind of doctor I would like taking care of me at my age.'”
Presuming that one geriatrician can care for 700 more patients like McLemore, the American Geriatrics Society figures this state should have 186 of these sub-specialists. It has 26.
That's based on its estimate that, of all Mississippians age 65 and older, more than 130,000 are vulnerable.

Shipley
“Sometimes, people just don't want to deal with them … because they move slower, they take their time, they can't hear you sometimes,” said Dr. Sonya Shipley, UMMC assistant professor of family medicine and a part-time geriatrics fellow.
“When a baby has an accident, it's cute; but when it's an adult, it can be off-putting to some.
“But, spiritually, viscerally, however you choose to phrase it, it's part of my life's work to impact the quality of care for our older adults.
“They've worked so hard; they paved the way for so many of us. I've met chefs, dancers, veterans, expert quilt-makers. They are such a wealth of knowledge, and they show graciousness and kindness in their willingness to share their knowledge with you.”
Compared to rest of the country, Mississippi's geriatric numbers may not sound tsunami-like. Worldatlas.com sets the state's total elderly population - approximately 428,000 - at 14.27 percent of all Mississippi residents. That's lower than the figure for about 34 other states.
“But Mississippi already has a low physician-to-patient ratio,” Meeks said. “It has a lack of access to health care. So the health of geriatric patients here may be poorer compared to those in other states with even greater geriatric populations.”
Those populations combined have created a nationwide need for 20,000 geriatricians, the AGS says; it has under 7,500.

Frank
“We aren't graduating geriatric medicine fellows fast enough,” said Dr. Kathy Frank, AGS board member, a PhD-level nurse and geriatric program administrator at the Indiana University School of Medicine.
“And we as a society don't acknowledge that we're aging. Look at the TV commercials. It's all about staying young. No one wants to talk about dying. About taking pills. People don't prepare for that flow.”
That flow “poses enormous challenges for the future of medical education,” the AAMC Reporter stated in April 2015.
“On top of this geriatrician shortage, the amount of education health-care providers receive does not prepare them to take care of an older adult or how to work together with the other professions to have a strong team care approach,” Frank said.
“Many older adults don't have advocates. People rally for kids; no one rallies for us old folks.”
‘IT’S A MOURNING PROCESS’
“Nothing says 'my doctor cares' more than them showing up at the front door,” Shipley said. “Unfortunately, it's a lost art.”
But not in the Division of Geriatrics. Periodically, Meeks alone makes home visits to at least a half-dozen patients.
These home visits for older patients are usually warranted when clinic visits are a “burden,” said Meeks, who also provides specialized Alzheimer's and dementia care at the MIND Center Clinic and TeleMIND Program.
Some of these patients are beset by dementia, as in the case of Jannie Leflore of Jackson.
As she lay on a home hospital bed during a visit last fall, she peered into her doctor's face, apparently with recognition. On a nearby wall someone had posted a handmade sign - “JANNIE G. LEFLORE HOUSE” - as if to reassure her. Beside it was photograph of the late husband she believes is still alive.
Some months earlier, it had taken her daughter, Janyce Leflore Jenkins, hours to coax her mother out of the car at a house she did not recognize - her own.
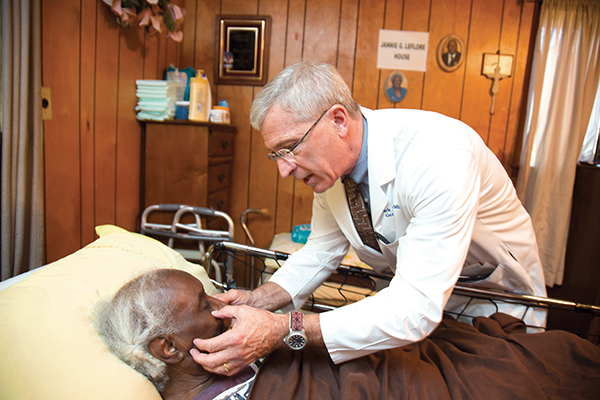
Dr. Mark Meeks offers the personal touch that home visits allow, during his examination of patient Jannie Leflore.
And that's why Meeks visits this home - to see a patient who knows that back room like the back of her hand, but doesn't recognize her own front door. Who knows her husband's name is William, but doesn't know he has died.
As geriatricians will tell you, older patients face issues that are rarer for their younger counterparts. Just as children aren't miniature adults, geriatric patients aren't middle-age adults on Medicare.
Not least among their nemeses are falls, the leading cause of injuries for older Americans. Every 19 minutes, an older adult dies from one, the National Council on Aging reports.
“Falls may be caused by four or five different issues,” Meeks said “That's when a geriatrician is probably called for.”
A geriatrician may be called for when families need guidance about whether to retire an older relative's car keys. Or how to stoke their own courage in the throes of caregiver burnout. Or where to find long-term care when they've been emotionally tapped out by home care.
“When your loved one has Alzheimer's, it's a mourning process,” said Sue Ann Meng, who leads a caregivers' support group, “because you're losing them a little bit at a time.”
Meng is a UMMC geriatrics social worker, licensed clinical social worker and mental health counselor whose experience with geriatric patients covers end-of-life diseases.
“The main thing is not the cure,” Meng said. “Because old age is not something you can cure. But that's not the way we think in health care. The attitude is, 'You need to fix it.'
“Instead, geriatricians are trained to think, 'What is it you want at this age?' And they respect those wishes.”
‘EVERYONE HAS KIDNEYS’
Skeptics say other clinicians are already addressing conditions elderly patients often confront, such as diabetes and hypertension, as are other health-care workers: nurses, physician assistants, occupational therapists, physical therapists and more.
Dr. Cynthia Brown, a national geriatrics expert, sees their point - to a point.

Brown
“Just because you're an older adult, that doesn't mean you need a geriatrician,” said Brown, professor in the Division of Gerontology, Geriatrics and Palliative Care at the University of Alabama at Birmingham School of Medicine.
“But 20 percent of older adults out there will really benefit from a geriatricians' care. We are trained in areas I didn't get as an internist. It's not all about age.
“There are people even at 65 who have multiple diseases; they will benefit from a geriatrician. It's about the burden of diseases. It's about complexity, which we are good at.”
Frank, the AGS board member, also said it's unrealistic to send everyone over 65 to geriatricians. “We need to focus on the high-risk patients instead. As a colleague of mine said, 'everyone has kidneys, but not everyone sees a nephrologist.'
“'But if they get sick enough, they see one.'”
Dr. Beverly “Gwen” Windham remembers, early in her career, a certain patient who was sick enough for a geriatrician. Now a UMMC professor of medicine with a geriatrics practice, she was an internal medicine resident at the time, taking a geriatrics elective under Meeks.

Windham
“There was a surgery patient over 80 who had bowel problems; she was also very confused,” Windham said. “Because of that and because of her age, the surgeons were reluctant to operate. I thought, 'She is not going to do well at all.'
“But Dr. Meeks said she needed the surgery. First, though, he made changes to her medications - and that took care of the confusion. She had surgery and went home.”
That case illustrates the predicament of the “prescription cascade” - using medications to treat side effects of other medications. Geriatricians are trained to be aware of such issues.
In medical schools, geriatrics rotations are elective in most internal medicine, family medicine and psychiatry programs. As for residents at UMMC, they're required to do one month of geriatric care.
In an attempt to fill in the gaps, many institutions offer geriatrics fellowships. Meeks directs UMMC's program, which is “100 percent clinical” and provides a year of subspecialty training to internal medicine or family medicine physicians, he said.
It's one of 130 similar programs in the country. But only about half of those programs' 383 positions have been filled. The Medical Center has trained about 10 fellows since its beginnings a few years ago. It's currently schooling three more geriatrics fellows, including Shipley.
With this specialized training, geriatricians can even help improve health care's bottom line: Stemming the costly prescription cascade is one thing that comes to mind, Meeks said.
In spite of such incentives, policy makers aren't paying enough attention, geriatricians say.
“From a legislative perspective, not so much,” Brown said. “For instance, no loan repayment programs are addressing this.” Even though geriatricians are among the lowest-paid physicians and reap relatively anemic reimbursements.
Then, there's research. “Even though older people use more resources and encounter the health system the most,” Windham said, “they are less studied than people in younger age groups.”
‘IF WE LIVE LONG ENOUGH’
Still, some medical schools and academic medical centers, including this one, are getting the message. “Internal medicine residents learn more about geriatrics than ever,” Windham said.
The training geriatrics fellows undergo has spilled over into other areas - to medical students, nurse practitioners and more. The geriatrics faculty has grown compared to several years ago, Windham said.
M1s now go on “senior visits” to nursing, assisted-living and private homes.
More of these kinds of approaches are needed to care for thousands more people like Jannie Leflore. The wall in place against the coming wave is low.
“But I really do believe changes are coming,” Shipley said. “I'm in geriatrics, and I think I'm a shining ray of sunshine,” she said with a laugh.
“If nothing else, people who have the power to make it happen will have a vested interest. If we all live long enough, we'll all get old.”


