Early detection vital to successful melanoma treatment
Published on June 01, 2017
NOTE: This article originally appeared in the June 2017 issue of CONSULT, UMMC's monthly electronic newsletter. To have CONSULT, and more stories like this, delivered directly to your inbox, click here to subscribe.

Breakthroughs in melanoma treatment that started in 2011 are continuing to bring hope to patients with metastatic disease, say doctors who specialize in treating the deadly skin cancer.

Brodell
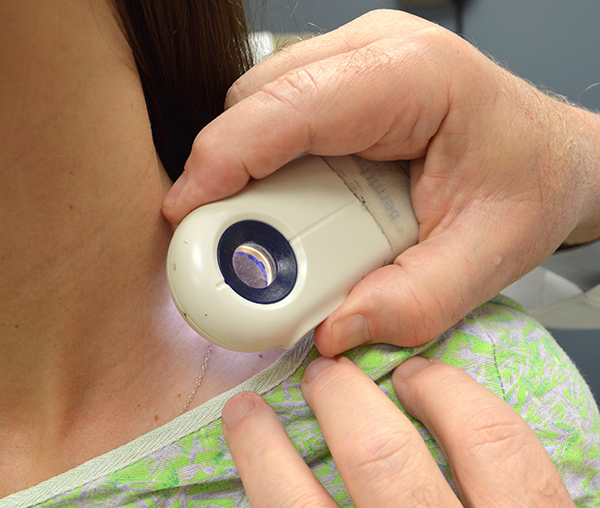
This cancer usually is associated with a change in a mole, said Dr. Robert Brodell, chair of dermatology. It's also the deadliest of skin cancers.
Caught early, melanomas often can be removed, curing the disease. Undetected, they can grow and spread to other organs.
Therapy after the cancer spreads, or metastasizes, once offered little hope, said Dr. Natale Sheehan, assistant professor of hematology/oncology and a medical oncologist who works with many melanoma patients.
“We've had so many drugs just explode on the scene since 2011,” she said. Those include immunotherapies and molecular-targeted therapies that have eclipsed chemotherapy as the standard of care.

Sheehan
Now, the UMMC Cancer Institute's interdisciplinary melanoma team has new options for patients with lymph node-positive melanomas, for example. And a recent study showed the two-year survival rate for patients on combined therapies was 64 percent versus 45 percent for those on a single-agent therapy.
The melanoma team includes dermatologists, medical and radiation oncologists, oncologic surgeons and many others who discuss each case and develop a treatment plan for each patient. Together, those specialists and others offer the state's only melanoma clinic.
“You can see all of us at one point in time and we can all develop a plan together to actively work toward treatment of each patient's disease,” Sheehan said.
“The complex treatment options for melanoma point out the advantages of visiting an interdisciplinary melanoma clinic like the one we have at UMMC,” Brodell said. “Dermatologists, oncologists, general surgeons and plastic surgeons work together to design the right treatment at the right time for each patient to offer the most hope for improvement in melanoma and sometimes even long-term remissions.”
Brodell and Sheehan still advise patients to know their own skin and see a doctor early when they notice changes.
“Many patients are still unaware of the importance of showing their doctor a mole that is new or changing,” Brodell said.
Better yet, take steps to avoid melanoma.
American Academy of Dermatology tips to help avoid skin cancers
• Wear broad-brimmed hats;
• Stay in the shade from 10 a.m. to 2 p.m. when ultraviolent rays are strongest;
• Wear sun screens with sun protection factors of SPF 30 or higher, also labeled broad spectrum UVA-UVB blockers;
• Reapply sun screens every two to three hours, especially if swimming or sweating;
• Wear sunglasses with UV protection;
• Check your body on the first day of every month for new growths, changing moles or sores that will not heal, and find a partner who can check your back;
• Show suspicious spots to primary care physicians or dermatologists; and
• Stop or do not start using tanning beds.


