Under the Rainbow, In the News - Fall 2014
Published on December 10, 2014
A kaleidoscope of significant news from Batson.
Preteen immunization is best bet against cancer later

Sarah Short, cytotechnologist in the Department of Pathology, prepares to examine a patient's Pap smear.
Experts at UMMC say parents should get children vaccinated against a sexually transmitted disease that can cause cancer in adulthood.
And although girls were the initial focus of the vaccine for human papillomavirus, or HPV, it’s just as important that boys are protected.
“Girls are getting their HPV from someone. They’re usually getting it from the boys,” said Dr. Rana El Feghaly, an infectious diseases specialist and assistant professor of pediatric infectious diseases.
“If you can prevent it in boys, then you can prevent it from being transmitted to girls.”
The HPV infection, the most common STD in the nation, is spread through genital skin-to-skin contact and sexual intercourse. And because the vaccine provides best immunity when given early – before sexual activity begins – the Atlanta-based Centers for Disease Control recommends children as young as 9 receive the immunization, given in three doses over a six-month period. The CDC recommends it for all children ages 11-12, boys through age 21, and girls through age 26.
The statistics in Mississippi are alarming. Just 12 percent of girls ages 13-17 complete the vaccine, the lowest rate in the nation, the CDC reports. The rate is 50 percent or higher in some other states.
Mississippi has a high rate of HPV infection, with an incidence of 8-10 new HPV-related cervical cancer cases per 100,000 population.
“It is critical for Mississippi physicians to understand and embrace the concept that the vaccine is useful in children who are not yet sexually active because of its effects years into the future, when the children grow into young adults who usually will become sexually active,” said Dr. Gailen Marshall, professor and division chief of allergy and immunology in the School of Medicine.
It’s sad, pediatrician Dr. Will Sorey said, that anyone would decline to protect their child against a disease that affects one in five Mississippians.
“This is like seat belts,” said Sorey, professor of pediatrics. “It’s just something you must do to protect yourself.”
Occupational therapist earns leadership kudos

Candice Barber is recognized for her thoughtfulness and hard work by Guy Giesecke.
When a coworker told Candice Barber about a dog left unattended for days in a car in the stadium parking lot adjacent to UMMC, the animal lover sprang into action.
Barber, an occupational therapist at Batson Children's Hospital, found out the dog's owners had a family member in the ICU at UMMC. Candice provided food, gift cards and gas cards for the family and helped with sleeping arrangements. She also made sure the dog was attended to during their stay.
She was recognized for her thoughtfulness and hard work by Children's CEO Guy Giesecke during the UHHS Leadership Meeting.
Ronald McDonald House celebrates 25 years

Groundbreaking Ronald McDonald House – Jackson
The Ronald McDonald House turned 25 this May, marking the occasion with a birthday celebration at the Cedars in Fondren where the man himself, Ronald McDonald, showed up.
Built on the UMMC campus with the help of four years of fundraising in 1989, the house is a "home away from home" for many families who have children requiring specialized medical care. Home-cooked meals, private bedrooms and playrooms for children are provided through the generosity of volunteers and donors.
Many UMMC staff and student groups regularly prepare and serve meals to the families, including Batson Children’s Hospital nurses, occupational therapy students and members of the American Medical Student Association.
The RMH is the cornerstone program for Ronald McDonald House Charities of Mississippi (RMHC MS). In 2000, RMHC MS began awarding grants to other non-profits that enhance the health and/or education of Mississippi children. To date, more than $165,000 has been given to Batson projects.
Fugate quads go home

The Fugate family takes one of their first photos together. Mom Kimberly holds Kayleigh Pearl, left, and Kenleigh Rosa, big sister Katelyn sits at center, while dad Craig holds Kristen Sue, left, and Kelsey Roxanne.
The Fugate quadruplets are finally all home.
The babies, all girls, were born Feb. 8, just shy of 13 weeks premature, to Kimberly Fugate, who was surprised at the announcement of the fourth baby.
“There are more feet.”
Those words, spoken by Fugate’s physician during delivery, first alerted her she was having quadruplets.
She and her husband, Craig, as well as the entire health-care team working on her case, believed she was having triplets.
Dr. James Bofill, professor of maternal fetal medicine, said the odds of quadruplets occurring without the use of fertility treatments are 1 in 729,000. But in the Fugates’ case, the odds are even smaller because their girls split from a single egg, meaning the siblings are identical.
“Those odds are incalculable,” Bofill said.
Kristen Sue and Kelsey Roxanne went home in early May, while Kenleigh Rosa and Kayleigh Pearl went home in late June.
Will Rogers, Variety charity award $25,000 to NICU

Todd Vradenburg, left, and Ron Krueger II, right, present a $25,000 grant to, from left, Dr. Sajani Tipnis, Tara Goddard, clinical director of the Newborn Center and Center for Maternal & Fetal Care, Billy Needham and Dr. Rick Barr.
The Will Rogers Institute and Variety, the Children’s Charity of the United States, awarded a $25,000 grant to the state’s only Level IV neonatal intensive care unit Aug. 22.
Todd Vradenburg, executive director of WRI, and Ron Krueger II, Variety board member and president and chief operating officer of New Orleans-based Southern Theatres, presented the check to Dr. Rick Barr, Suzan B. Thames Professor and Chair of Pediatrics, Dr. Sajani Tipnis, associate professor of neonatology and medical director of the NICU, and Billy Needham, Newborn Center nurse educator, who applied for the grant.
“We’re so happy to have been able to work with Variety and bring this grant together,” Vradenburg said.
The funds purchased two Sentec Transcutaneous CO2 monitors along with several months’ worth of supplies. The monitor reports CO2 levels and other respiratory trends on a minute-to-minute basis via a probe placed on the baby’s chest, avoiding the need for repeated blood tests.
“We have many small patients where vascular access is an issue,” Tipnis said. “We have outstanding staff that does a very good job, but sometimes you just can’t get that line. In those cases, these machines are going to help us non-invasively monitor these babies.”
UMMC is among 14 recipients of grant money from the Will Rogers Institute this year. Last year, WRI committed $400,000 in grants for neonatal intensive care units to purchase much-needed equipment.
Procedure repairs hearts without opening children’s chests

Dr. Makram Ebeid holds patient Wyatt Stout, 2, of Pass Christian during a visit following Wyatt’s heart-repair procedure done via catheter.
Moms and dads of babies born with what’s known as a “hole” in their heart usually brace themselves for open-heart surgery, the accepted route to fixing the life-threatening defect.
But a significantly less invasive procedure that a University of Mississippi Medical Center pediatric cardiologist carries out in a catheterization lab is giving children and parents a new option: A simple overnight hospital stay and a regular Band-Aid on the children's leg in lieu of a line of chest stitches.
Sixteen children have successfully undergone Dr. Makram Ebeid’s procedure to plug a perimembranous ventricular septal defect in their heart’s lower half by transporting the plug on a catheter that is advanced through the child’s leg. It’s a transformational development borne of clinical trials that could, in time, replace the decades-old standard of surgery requiring at least a three- to five-day stay and post-op care in the pediatric cardiac care unit, Ebeid said.
“It makes so much sense that this is the right thing to do,” said Ebeid, professor of pediatric cardiology and director of the Pediatric Catheterization Lab.
If more parents only knew they could avoid open-heart surgery on their babies or toddlers, many would jump at the chance, said Dr. Jorge Salazar, professor of pediatric heart surgery and co-director of the Children’s Heart Center.
A ventricular septal defect is an opening in the septum wall that separates the heart’s left and right ventricles. That congenital flaw is almost always repaired during open-heart surgery.
Ebeid, however, has developed a trans-catheter approach. Guided by X-ray imaging, Ebeid threads a wire through a tiny hole in the patient’s leg and into a blood vessel or artery. The wire is guided to the patient’s heart, and the cardiologist passes instruments over the wire that are used to make repairs, such as a plug to seal an opening in the heart or replacement valves to relieve those that no longer work.
Ceremony honors leaders in children’s nursing

Dr. Janet Harris, left, associate dean for practice and community engagement in the School of Nursing, presents the 2014 Nurse of the Year Award to Denise Adams, a nurse in the pediatric emergency department.
Batson’s leading nurses took home many of the top honors at the 2014 Excellence in Nursing Award ceremony in May.
Awardees include: James Polson, D.N.P., director of clinical operations for the Division of Cardiothoracic Surgery, Advanced Practice Nurse of the Year; Dennis Demesa, R.N., Clinical Practice Nurse of the Year; Adyn Dancy, R.N., Nurse Rookie of the Year; Denise Adams, B.S.N., R.N., Nurse of the Year; Pam Farris, R.N., Nurse Manager of the Year; and Terri Gillespie, chief nursing executive officer and former chief nursing officer for Children’s of Mississippi, Nurse Administrator of the Year.
Emergency teams aid in tornadoes' aftermath

Damaged interior of Winston County Medical Center in Louisville
Tornadoes that ripped through the state in late April put UMMC into action to help fellow Mississippians in need.
The team of medical and emergency professionals is part of a statewide network coordinated from the Medical Center.
Knowing traumatic injuries were likely, leaders activated UMMC’s Emergency Operations Plan, which clears and readies adult and pediatric trauma rooms, emergency department capacity and operating rooms.
Two 16-member teams, including one pediatric transport team, deployed from UMMC to support search-and-rescue efforts in Tupelo. They traveled with an eight-bed mobile field hospital contained in an 18-wheeler truck. The unit is essentially an emergency room on wheels, part of a joint asset of the State Department of Health and UMMC.
Aubrey Pepper, perioperative nurse educator at Batson Children’s Hospital, noted the tenderness operating room staff showed toward storm victims.
Staff members bought lunch for the families of victims, purchased hair brushes and washed the children’s mud and debris-filled hair, Pepper wrote in an email. Staff took extra care to bathe the children while they were asleep so the children would wake up from their surgeries clean, comfortable and at lower risk for infections.
“I have seen this type of extra effort time and time again from the Batson surgery team, but rarely are they recognized for their efforts,” Pepper wrote. “Due to the nature of perioperative services, these staff are unseen by families, but their exceptional work has long-lasting effects.”
New pediatric specialists added to Children's faculty
To meet the growing needs of its patients, Children’s of Mississippi added the following specialists to its staff recently. For more information about Children's of Mississippi services or to make an appointment, visit www.ummchealth.com/children.
Marcus Lee, M.D., Neurology
Melissa Rhodes, M.D., Hematology-Oncology
Eric Dec, M.D., Genetics
Uwe Blecker, M.D., Ph.D., Gastroenterology
Zach Cannon, M.D., Ambulatory-Grenada Lakes
Holly Dawson, M.D., General Pediatrics
Austin Harrison, M.D., General Pediatrics
Salwa Gendi, M.D., Cardiology-Tupelo
Christian Paine, M.D., Palliative Medicine
Atul Poudel, M.D., Nephrology
Anza Stanley, M.D., Ambulatory
Spencer Sullivan, M.D., Hematology-Oncology
Kathryn Thomas, M.D., Ambulatory-Grenada
Lamar Davis, M.D., Neurology
Michael Foster, M.D., Emergency Medicine
Dustin Sarver, Ph.D., Child Development
Nina Sarver, Ph.D., Child Development
Divya Shakti, M.D.Cardiology
Christopher Bean, M.D. , Surgery-Urology
Damon A. Darsey, M.D., Emergency Medicine
Sabahat Afshan, M.D., Nephrology
Sophie Lanciers, M.D., Gastroenterology-Endocrinology
New law advances cannabis-derived epilepsy treatment
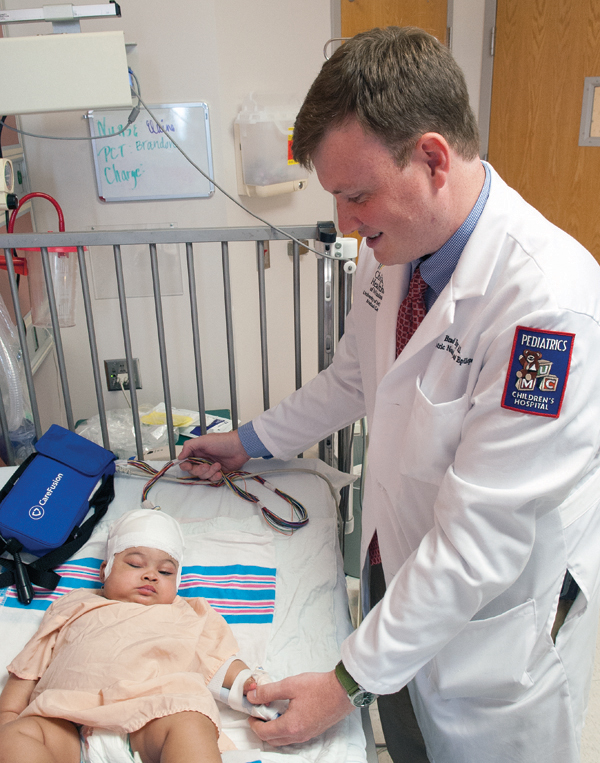
Dr. Brad Ingram, assistant professor of pediatric neurology, examines epilepsy patient Olivia Edwards.
The Mississippi Legislature passed legislation in April approving the University of Mississippi Medical Center to dispense cannabidiol (CBD) oil, a non-psychoactive constituent of the cannabis plant that may have anti-seizure activity, for the treatment of epileptic seizures in children.
The Harper Grace’s Law is named for Harper Grace Durval, a 2-year-old Batson patient who suffers from a rare form of epilepsy called Dravet Syndrome.
Unlike “medical marijuana” that is legal in some states, the oil that is the subject of Harper Grace’s Law is extracted from cannabis and is orally administered, not smoked. In addition, the specially processed oil contains a very low amount of tetrahydrocannabinol, or THC, the principal psychoactive constituent of the cannabis plant.
Rigorous and formal research studies in humans need to be conducted to establish the oil’s effectiveness and safety.
Before patients can receive the potential treatment in a carefully controlled clinical trial in Mississippi, major regulatory requirements still exist and meeting them could take a year or more.
The requirements include securing federal regulatory approval to grow, process and transport the variant of low-THC, high-CBD marijuana from which the oil is extracted. The National Center for Natural Products Research at the University of Mississippi School of Pharmacy in Oxford has recently gained approval from two federal agencies to grow a certain quota of the particular strain.
Any such clinical trial established at UMMC would initially involve children with refractory or more serious types of epilepsy. There are no current plans to study the effectiveness of CBD oil or smoked marijuana on seizure activity in adults. Nor do UMMC neurologists feel that smoked marijuana – whether medical or recreational – currently has a place in treating epilepsy.
Dedication of Wall of Heroes honors pediatric organ donors

Jackie McInnis of Mount Olive has her photo taken next to the newly dedicated Wall of Heroes at Batson Children’s Hospital, which honors pediatric organ donors including her son, Gary Lenzie McInnis.
The “Wall of Heroes” honoring pediatric organ donors at the University of Mississippi Medical Center was dedicated on a June morning at Batson Children’s Hospital.
The wall is a joint effort of the Mississippi Organ Recovery Agency, the Mississippi Lions Eye Bank and the state’s only children’s hospital to commemorate the lives of children who gave the gift of life to others.
Video available at youtube.com/batsonhospital, search channel for “MORA”
Children's Hospital patient wins Orlando Dream Giveaway

Rob Armour, left, presents Grant Wilcher with a $1,000 Friends of Children’s Hospital CheckCard. Other members of the Wilcher family are, from left, sister Alex, dad Jimmy and mom Lori. Older brother Bo is not pictured.
Twelve-year-old Batson patient Grant Wilcher of Union and his family were announced as the winner of the BankPlus Orlando Dream Giveaway in July.
“We’re going to Disney World!” Grant said after the announcement.
Wilcher and his family were presented a vacation package worth more than $10,000 that includes round-trip airfare, ground transportation, five days’/four nights’ accommodation at Walt Disney World’s Polynesian Resort, tickets to Walt Disney World parks and a $1,000 BankPlus Visa gift card. They plan to take the trip during the Thanksgiving holiday.
The Wilchers qualified for the contest because of Grant’s stay at Batson Children’s Hospital for a neurological condition that causes headaches and other symptoms.
The Orlando Dream Giveaway contest was open to any family that had a child stay at Batson Children’s Hospital for at least one night between March 15, 2013 and June 30, 2014. Eligible families participated through Facebook and mail.
In addition to the Batson patient family, any holder of the BankPlus Friends of Children’s Hospital Visa CheckCard who used the card between March 15, 2014 and June 30, 2014 was automatically entered into the contest for a second, identical grand prize. DeDe Franciskato of Madison won that prize.
First issued in 2011, BankPlus has issued more than 8,400 Friends of Children’s Hospital Visa CheckCards. This year alone, these cards will be swiped more than one million times. With each swipe, BankPlus donates money to Friends.
“What this means is that in less than three years, this CheckCard program will raise over half a million dollars for Friends to help Batson Children’s Hospital,” said Rob Armour, BankPlus chief marketing and business development officer, who also serves as president of the Friends of Children’s Hospital board.
Pediatric nurse garners recognition for achievement

Hailey Moore
The UMMC Awards Team recognized Hailey Moore, registered nurse in the pediatric surgery suite, during a July leadership meeting.
Moore spent two hours of her own time consoling and assisting a visibly upset father in the waiting room of the surgical floor so that he "wouldn't have to be alone." Moore stayed with him until another family member joined him in the waiting room.
Pediatric palliative care establishes accredited fellowship
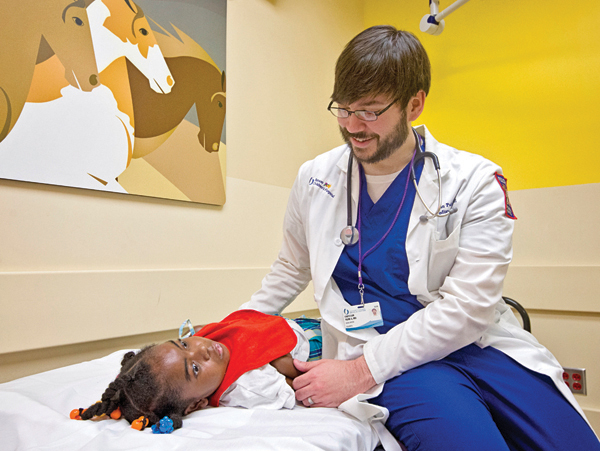
Dr. Christian Paine, assistant professor of pediatrics, examines Tisheanna Phinizee, 8, of Columbus.
The Division of Pediatric Palliative Care recently became one of only 10 programs nationwide to offer an accredited pediatric-dedicated fellowship in hospice and palliative medicine. It graduated its first fellow in July.
After completing his fellowship, Dr. Christian Paine became eligible for certification by the American Board of Pediatrics in hospice and palliative medicine.
Because completing a fellowship is the only pathway to board certification in this discipline, Dr. Rick Boyte, professor and chief of pediatric palliative care, believes getting the accreditation lends the pediatric palliative care program credibility.
“There are many children’s hospitals out there with palliative care services doing a great job taking care of patients, but I think having a fellowship shows an additional commitment and level of expertise,” Boyte said. “I’m very proud of the fact that we’re one of the few because I think it shows a commitment to expanding, to growing, but especially to maintaining the level of expertise.”
Paine is one of only 14 potential graduates to enter the medical work force with this level of training and expertise.
Boyte is hopeful the one-year fellowship will help grow the pediatric palliative care program by encouraging pediatric residents to come to UMMC for the one-year fellowship and then stay and join the staff, much like Paine, who became an attending physician with the program in July.
The fellowship is one of only four offered in pediatrics at UMMC, with others in pediatric intensive care, neonatal intensive care and hematology-oncology. The Accreditation Council for Graduate Medical Education offers the certification and is the only organization of its kind that evaluates residency and fellowship programs throughout the United States.
Children’s Safety Program: new report underscores importance of buckling up

Liz Foster
A new report on possible reasons why more teens die in motor vehicle crashes than from any other cause of death is sounding alarm bells for Children's of Mississippi’s safety and community outreach staff.
Published in June by Safe Kids Worldwide, “Teens in Cars” is an effort to find ways to reduce the number of teens killed in cars, currently approximately 2,500 per year. In half of the fatal crashes the teen was not wearing a seat belt.
“We need to encourage everyone to buckle up on every ride, every time,” said Elizabeth Foster, manager of the Safety and Community Outreach Program at Children’s of Mississippi, the health system anchored by Batson Children’s Hospital and the lead agency for Safe Kids Mississippi.
The report is based on answers gathered in a national survey of 1,000 teen passengers and drivers ages 13 to 19 and looks at why they aren’t buckling up, what their distracted driving habits are and how they behave when they feel unsafe in a car.
Foster and her staff, along with community partners, have been tackling the problem in Mississippi through a monthly Drivers IMPACT (Improving Motor Vehicle Practices Among Community Teens) class designed to educate teens on the skills needed to be safe drivers and the realities of driving dangerously. Nearly 300 teenagers have participated in this program since 2011.
“It only takes one time to forget to buckle up for a life to be changed forever,” Foster said.
Researchers find detectable HIV in “Mississippi Baby”

Dr. Hannah Gay
In early July 2014, the child known as the “Mississippi baby” who had been in remission from an HIV infection was discovered to have detectable levels of HIV after more than two years of not taking antiretroviral therapy and without evidence of virus.
“I have been involved with the child’s care since birth and I am deeply saddened by this turn of events,” said Dr. Hannah Gay, professor of pediatric infectious diseases. “It was a punch in the gut to see these test results last week. I know intellectually the child is going to be fine, but with a lifetime of medicines ahead, it’s more than just a little disappointing.”
The child was born to an HIV-infected mother who was not diagnosed with HIV infection until the time of delivery. Because of the high risk of HIV exposure, Gay started the infant at 30 hours of age on a triple-drug antiretroviral treatment traditionally used for prophylaxis. Testing confirmed that the baby had been infected with HIV.
The baby continued on antiretroviral treatment until 18 months of age, when the child was lost to follow-up care and no longer received treatment. Five months later, blood samples revealed undetectable HIV levels and no HIV-specific antibodies. The child continued to do well in the absence of antiretroviral medicines and was free of detectable HIV for more than two years.
The child has now been placed on standard doses of medication for HIV infection.
“I am confident the child will live a long and healthy life and while, as a clinician, I am more than disappointed for the child, I am hopeful for all researchers still looking for a cure,” Gay said. “The search for a cure is like a giant puzzle being put together and the things that have been learned from this case have contributed many pieces to the puzzle. Unfortunately, it wasn’t the final piece.”
Friends of Children’s Hospital begins MiracleHome

Cutting the first board for framing the 2014 MiracleHome are, from left, Mark Petro, Ridgeland Chamber of Commerce president, Gene McGee, Ridgeland mayor, Leigh Reeves, Friends president, George Gunn, Trustmark executive vice president and Scott Shoemaker, builder.
After a three-year hiatus, the MiracleHome project is back.
Friends of Children’s Hospital broke ground in July on the 2014 Batson MiracleHome, presented by Trustmark National Bank.
Co-created in 2003 by Friends of Children’s Hospital and the Home Builders Association of Jackson (HBAJ), the Batson MiracleHome quickly became one of Friends’ largest fundraisers. Friends and the HBAJ work with a volunteer builder to construct the home. This year’s builder is Scott Shoemaker of Shoemaker Homes.
The home is located in the Enclave subdivision in Ridgeland. Only 6,000 tickets are being sold at $100 each for the Dec. 6 giveaway date. For more information or to purchase a ticket, call 1-877-AHOME-2U.
Partnership transforms Children's behavioral and mental health

Gov. Phil Bryant addresses a crowd at an announcement of the Children's Collaborative, a partnership between UMMC and Mississippi Children's Home Services. Joining him are Dr. Susan Buttross, front row left, Dr. John Damon, front row right, CEO of MCHS, and employees of MCHS and Medicaid.
The Children’s Collaborative, a transformative partnership announced in the spring between UMMC and Mississippi Children’s Home Services (MCHS), envisions a state-wide, integrated behavioral and mental health-care system that will ultimately reduce costs and improve quality of care.
Supported by a $5 million grant awarded by the Center for Medicare and Medicaid Services and the Mississippi Division of Medicaid, this unique public/private partnership is the first of its kind in the nation.
According to Dr. Susan Buttross, professor of pediatrics and chief of the Division of Child Development and Behavioral Pediatrics, one in five children suffers from a mental or behavioral health problem, and less than 20 percent receive treatment.
During the next 18 months, the Children’s Collaborative will be working to ease the burden placed on the caregiver by partnering with the child’s pediatrician, often the first point of contact for the family when seeking behavioral health services.
UMMC’s Center for the Advancement of Youth will serve as a gateway for families to enter the Children’s Collaborative’s system of coordinated care.
Following a comprehensive assessment at the Center for the Advancement of Youth, children served through the Children’s Collaborative are then seamlessly directed to various UMMC pediatric specialists and/or to community-based behavioral health services provided by MCHS.
MCHS will offer this behavioral health care in the home and community of the child in one of the 11 outpatient offices located around the state.
Over the course of the project, the Children’s Collaborative also plans to develop a telehealth network within these 11 offices to help these children and families access other UMMC pediatric sub-specialty services, such as endocrinology and pulmonology.


