A Better Model to Integrate Physician Leaders
Good morning!
My day started earlier than usual with a 4 a.m. session of Leadership Rounds this morning. A diverse group of about 60 leaders broke into smaller groups for visits to the adult tower, the ICUs, the ED and ORs, Wiser and Children’s. In the 2½ years we’ve been making these visits to the “front lines,” my sense is the level of engagement on both sides – the clinical staff and those rounding – has never been higher. As we kick off Patient Safety Awareness Week next Monday, I want to salute our nurses, patient care techs, therapists, housekeepers, unit secretaries, students, physicians and others who are all working hard together to keep our patients safe.
 Today, however, my focus is on physicians. Perhaps it goes without saying – physicians are crucial players in the life of our academic medical center. They are leaders of the health care team and leaders of our education mission in medicine. They are in the forefront of our growing efforts in clinical research. And as we look to build relationships with other health care entities in the marketplace, physicians are at the table as strategic leaders and negotiators.
Today, however, my focus is on physicians. Perhaps it goes without saying – physicians are crucial players in the life of our academic medical center. They are leaders of the health care team and leaders of our education mission in medicine. They are in the forefront of our growing efforts in clinical research. And as we look to build relationships with other health care entities in the marketplace, physicians are at the table as strategic leaders and negotiators.
During the last year, based on input from many quarters, I have given much consideration to the desire and need for greater physician involvement in both strategic and operational activities of our health care mission. The time is right to move in this direction. We are making major decisions on such topics as our clinic space, surgical services, inpatient priorities and strategic health care partnerships, and we need a better model to integrate the voice of the physician.
To this end, I have been putting in place a number of initiatives in the clinical enterprise. The first is the appointment of a number of senior physicians to work with health system administrators in a dyad or shared leadership model in the adult setting. This model has worked well in the pediatric setting and elsewhere. These new appointments include:
- A Chief Operations Physician who will partner with the adult hospital CEO on such issues as capacity management, length of stay and continuity of care. Alan Jones, professor and chair of emergency medicine, has assumed this role.
- A Chief Network Physician who will partner with administrators on affiliations, joint ventures and other relationships with external entities. George Russell, professor and chair of orthopaedic surgery, has assumed this role.
- A Chief Ambulatory Physician who will partner with the Chief Ambulatory Officer for adult services on clinic operations with such goals as improving efficiency, service and the faculty practice plan. Scott Stringer, professor and chair of otolaryngology and communicative sciences, has transitioned into this role from his previous position as Chief Physician Executive.
Each of these physician-leaders will retain their responsibility as department chair and their respective dyad will report to the Health System CEO-Associate Vice Chancellor for Clinical Affairs dyad (Kevin Cook and Dr. Charles O’Mara, respectively).
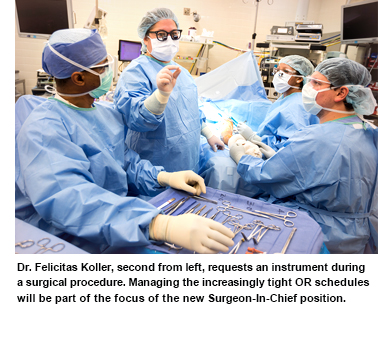
Also, in the next few months, I will move forward with the creation of a Surgeon/Physician in Chief for Adult Operative Services. With the appropriate administrative partner, this leader will serve as a single point of focus for all matters relating to surgery, in addition to serving as a practicing surgeon/physician. I’ve asked a number of stakeholders to define the scope and authority of this new position and then we will conduct an internal search with the goal of filling the position in the coming months.
Finally, I have established one new monthly meeting to enhance communication and strategic decision-making. This new group will be named the Clinical Cabinet and will include physician leadership, senior health system administrators and other stakeholders needed to identify and evaluate issues, come to consensus, and present alternatives for final decision.
I hope the initiatives outlined above will go a long way toward improving communication, decision-making and engagement of our physicians in addressing the vital interests of our clinical enterprise. The health care landscape is changing – What an understatement! – and we must make thoughtful, fully vetted decisions in real time to position ourselves for success. I’m confident we will, on our shared journey to A Healthier Mississippi.

